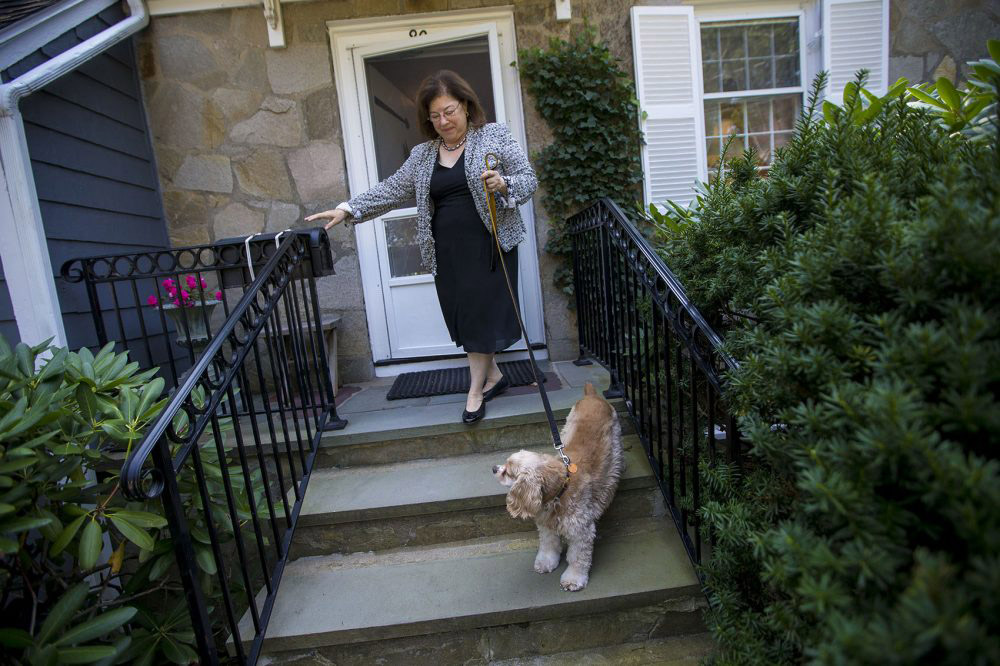In April this 12 months, Katie Herzog checked right into a Boston instructing hospital for what turned out to be a nine-hour-long again surgical procedure.
This story is a part of a partnership that features WBUR, NPR and Kaiser Health News. It might be republished totally free. (details)
The 68-year-old consulting agency president left the hospital with a prescription for Dilaudid, an opioid used to deal with extreme ache, and directions to take two tablets each 4 hours as wanted. Herzog took near the complete dose for about two weeks.
Then, nervous about habit, she started asking questions. “I said, ‘How do I taper off this? I don’t want to stay on this drug forever, you know? What do I do?’” Herzog mentioned, recalling conversations together with her numerous suppliers.
She mentioned she by no means acquired a transparent reply.
So she turned to Google to attempt to determine how to wean herself off the Dilaudid. She finally discovered a Canadian Medical Association information to tapering opioids.
“So I started tapering from 28 [milligrams], to 24 to 16,” Herzog mentioned, scrolling by a pocket diary with pink cardinals on the duvet that she used to maintain monitor.
About a month after surgical procedure, she had a follow-up go to together with her surgeon. She had reached the tip of her self-imposed tapering path the day earlier than and on the physician’s, she recollects feeling fairly sick.
“I was teary, I had diarrhea, I was vomiting a lot, I had muscle pains, headache, I had a low-grade fever,” Herzog recalled.
The surgeon thought she had a virus and instructed her to see her internist. Her internist got here to the identical conclusion.
She went dwelling and suffered by 5 days of what she got here to comprehend was acute withdrawal, and two extra weeks of fatigue, nausea and diarrhea.
“I had every single symptom in the book,” Herzog mentioned. “And there was no recognition by these really professional, senior, seasoned doctors at Boston’s finest hospitals that I was going through withdrawal.”
Email Sign-Up
Subscribe to KHN’s free Morning Briefing.
Herzog didn’t identify any of the suppliers who had one thing to do together with her ache administration or missed indicators of withdrawal. She mentioned she sees this as a system-wide downside. Herzog did share medical information that assist her story. After the withdrawal, she didn’t crave Dilaudid and he or she manages any lingering ache with Tylenol. She has since returned to her suppliers, who’ve acknowledged that she was in withdrawal.
Not An Isolated Incident
Herzog’s story is one medical doctors are listening to increasingly more. “We have many clinicians prescribing opioids without any understanding of opioid withdrawal symptoms,” mentioned Dr. Andrew Kolodny, director of Physicians for Responsible Opioid Prescribing and co-director of the Opioid Policy Research Collaborative at Brandeis University’s Heller School. One motive, Kolodny mentioned, is that medical doctors don’t understand how rapidly a affected person can grow to be depending on medication like Dilaudid.
Sometimes that dependence results in full-blown habit. About half of street drug users say they switched to heroin after prescribed painkillers grew to become too costly.
Now, a handful of medical doctors and hospital directors are asking, if an opioid habit begins with a prescription after surgical procedure or another hospital-based care, ought to the hospital be penalized? As in: Is habit a medical error alongside the traces of some hospital-acquired infections?
Writing for the weblog and journal Health Affairs, three physician-executives with the Hospital Corporation of America argue for calling it simply that.
“It arises during a hospitalization, is a high-cost and high-volume condition, and could reasonably have been prevented through the application of evidence-based guidelines,” write Drs. Michael Schlosser, Ravi Chari and Jonathan Perlin.
The authors admit it will be onerous for hospitals to watch all sufferers given an opioid prescription within the weeks and months after surgical procedure, however they are saying hospitals must attempt.
“Addressing long-term opioid use as a hospital-acquired condition will draw a clear line between appropriate and inappropriate use, and will empower hospitals to develop evidenced-based standards of care for managing post-operative pain adequately while also helping protect the patient from future harm,” mentioned Schlosser in an emailed response to questions.
Kolodny mentioned it’s an concept price contemplating.
“We’re in the midst of a severe opioid epidemic, caused by the over-prescribing of opioids,” Kolodny mentioned. “Putting hospitals on the hook for the consequences of aggressive opioid prescribing makes sense to me.”
Potential Addiction Vs. Pain Management Awareness
But penalizing hospitals for sufferers who grow to be hooked on opioids conflicts with funds tied to affected person satisfaction surveys. Hospitals that don’t adequately handle sufferers’ ache could lose cash for low affected person satisfaction scores. In response to the opioid epidemic, affected person surveys are shifting from questions like, “Did the hospital staff do everything they could to help you with your pain?” to questions that emphasize talking to patients about their pain. But physicians should still prescribe extra, fairly than fewer, opioids to keep away from complaints from dissatisfied sufferers.
“This is a real concern that patients who may feel that their pain is under-managed may take that out in these patient report cards,” mentioned Dr. Gabriel Brat, a trauma surgeon at Beth Israel Deaconess Medical Center who research the usage of opioids after surgical procedure at Harvard Medical School.
Most sufferers go away the hospital with extra ache meds than they want. Studies show that between 67 and 92 p.c of sufferers have opioid tablets left over after frequent surgical procedures.
One motive which will contribute to over-prescribing is that sufferers range rather a lot. Brat mentioned about 10 p.c of sufferers want intense ache administration, but it surely’s tough to determine who might be that 10 p.c.
“Many surgeons are still prescribing opioids for the subset of patients that have higher requirements, as opposed to for the majority of patients who are taking a very small percentage of the pills that they are prescribed,” Brat defined.
There are not any agency pointers for which opioids to prescribe after surgical procedure, at what dose or for a way lengthy. The CDC launched opioid prescribing pointers for power ache in 2016, but it surely included solely transient references to acute ache.
Some opioid prescribing steerage for surgeons is rising. A study printed in September reviewed surgical information for 215,140 sufferers. It discovered that the optimum opioid prescription following basic surgical procedure is between 4 to 9 days.
This story is a part of a reporting partnership with NPR, WBUR and Kaiser Health News.
Martha Bebinger, WBUR: [email protected]”>[email protected], @mbebinger
Related Topics Health Industry States Hospitals Massachusetts Opioids src=”http://platform.twitter.com/widgets.js” charset=”utf-Eight”>