This story is a part of a partnership that features KQED, NPR and Kaiser Health News.
This story might be republished totally free (details).
Many of Ron Fleming’s fellow troopers have spent the previous 5 many years attempting to neglect what they noticed — and did — in Vietnam.
But Fleming, now 74, has spent most of that point attempting to carry on to it. He’s by no means been as proud as he was when he was 21.
Fleming was a door gunner within the conflict, hanging out of a helicopter on a strap with a machine gun in his arms. He fought within the Tet Offensive of 1968, generally for 40 hours straight, firing 6,000 rounds a minute. But he by no means gave a lot thought to catching a bullet himself.
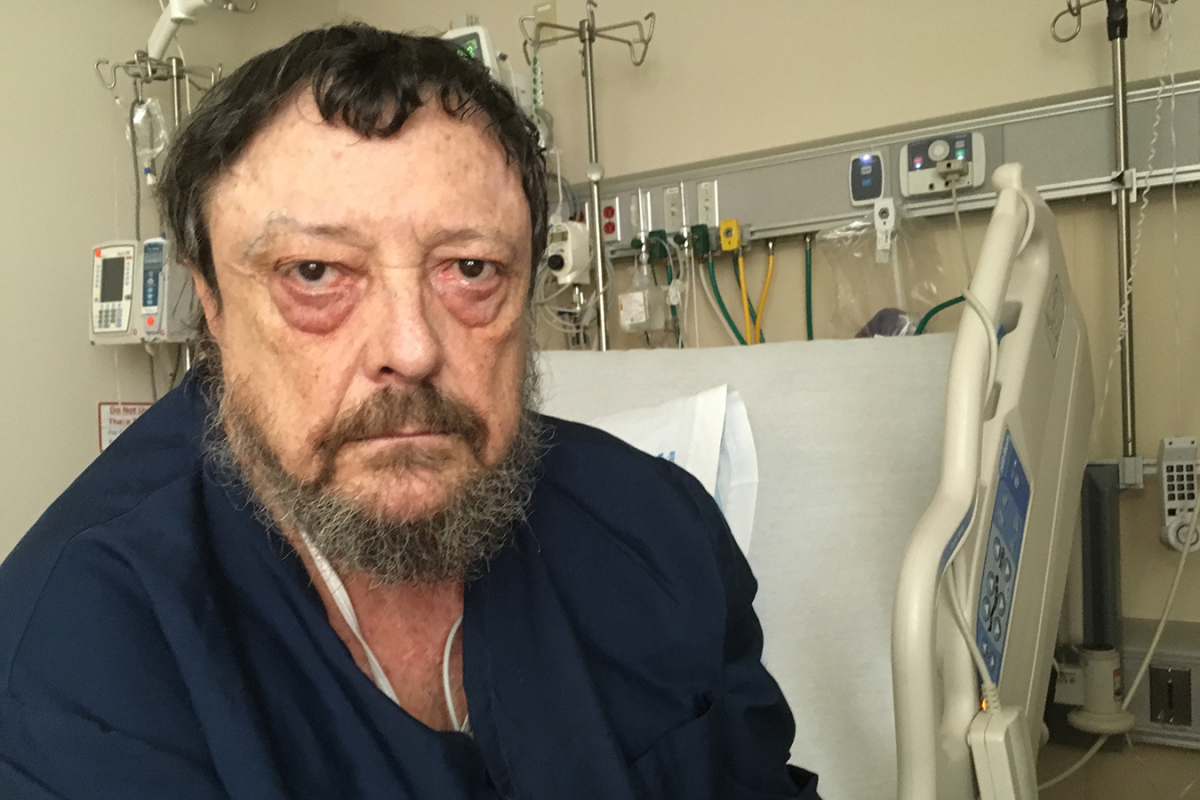
“At 21, you’re bulletproof,” he mentioned, as he sat on the sting of his hospital mattress on the San Francisco VA Medical Center. “Dying wasn’t on the agenda.”
Now it’s. Fleming has congestive coronary heart failure and arthritis, and his bronchial asthma assaults usually land him within the hospital. Ten years in the past, he was recognized with post-traumatic stress disorder (PTSD), which makes him fast to anger and hypervigilant, as if he’s nonetheless in that helicopter.
Fleming’s bodily and psychological well being signs, mixed along with his navy historical past, are a problem to the VA’s palliative care crew, which is coordinating his care as his well being deteriorates. It is a problem they’re dealing with extra usually as Vietnam veterans age and develop life-threatening sicknesses.
For some veterans, the stoicism they honed on the battlefield usually returns full-force as they confront a brand new battlefront within the hospital, making them much less keen to confess they’re afraid or in ache, and fewer keen to just accept remedy. Other vets, with PTSD, are much more reluctant to take pain-relieving opioids as a result of the medication can truly make their signs worse, triggering scary flashbacks.
About 30 % of Vietnam vets have had PTSD of their lifetime, the very best fee amongst veteran teams, in line with the U.S. Department of Veterans Affairs’ National Center for PTSD. Their fee is larger due to the distinctive fight circumstances they confronted and the adverse reception lots of them obtained once they returned house, in line with quite a few studies.
Email Sign-Up
Subscribe to KHN’s free Morning Briefing.
Since the conflict, many vets have developed coping methods to maintain disturbing recollections and different PTSD signs at bay. But dealing with a terminal sickness — the extreme ache of most cancers, the nausea of chemotherapy or the breathlessness of coronary heart failure — can drain their power a lot that they’re unable to keep up their psychological defenses. Vets beforehand recognized with PTSD can slip out of remission, and a few might expertise it for the primary time.
“They’re so distracted trying to cope with their physical symptoms that they might have flashbacks,” mentioned VJ Periyakoil, a palliative care doctor on the VA Palo Alto Health Care Center and director of palliative care training at Stanford University. “War memories start coming back; they start having nightmares.”
Gasping for breath can induce panic for anybody, however it will possibly make vets really feel as threatened as they did in a fight zone, mentioned Eric Widera, director of hospice and palliative care on the San Francisco VA and professor of geriatrics on the University of California-San Francisco.
That’s what occurs to navy vet Earl Borges, who logged 240 24-hour river patrols in Vietnam with three different males on a plastic boat, always in search of enemy troopers within the brush.
Since then, he’s been startled by loud noises and fast-moving shadows. Now, at age 70, Borges has amyotrophic lateral sclerosis (ALS) and persistent obstructive pulmonary illness, or COPD, which may intensify the anxiousness from his PTSD.
If he lies down with out his respiration machine, he panics, then hyperventilates.
“I have to talk him through it, tell him he’s OK, ‘just breathe,’” mentioned his spouse, Shirley Borges, 67.
Earl Borges performed river patrols in Vietnam. Now 70, the signs from his amyotrophic lateral sclerosis and persistent obstructive pulmonary illness can intensify the anxiousness he experiences because of PTSD. (Courtesy of Shirley Borges)
Borges in 1967 earlier than deploying for service on a guided missile destroyer that performed missions off the coast of Vietnam. The following yr, he served on a ship patrolling Vietnamese rivers. (Courtesy of Shirley Borges)
They each say Earl’s PTSD is beneath management — so long as he doesn’t speak in regards to the conflict — and his ALS is progressing very slowly, with out ache.
But for sufferers who’re in extreme ache, the go-to remedy is opioids, which may additionally make PTSD signs worse. This forces vets to decide on between bodily ache and psychological anguish.
“Oftentimes, pain medications like morphine or oxycodone make some people feel a little bit fuzzy,” Widera mentioned. “That may contribute to that feeling of loss of control.”
That’s why Periyakoil isn’t stunned when vets refuse ache drugs.
“‘Don’t you try and give me none of those narc pills, doc,’” she recalled certainly one of her sufferers saying whereas he grimaced in ache.
Some vets additionally refuse medicine as a result of they really feel as in the event that they deserve the ache.
“We see a lot of feelings of guilt over what they’ve seen and done during their experience in Vietnam,” Widera mentioned, “and they don’t want to blunt that.”
At the tip of life, this sense of guilt is amplified as vets look again and evaluate their lives and, maybe, ponder the results of their actions within the line of obligation. This is even true for vets like Fleming, whose overriding feeling about his service is pleasure.
“Sometimes I think that now I’m being paid back for all the men I killed. And I killed a lot of them,” mentioned Fleming, who has not required opioids for his situation, however has declined different drugs.
“If there is a judge, I figure I’m going to hell in a handbasket,” he mentioned.
Watching vets select to endure their ache might be arduous for households, in addition to for palliative care medical doctors and nurses. Just like troopers, medical doctors hate doing nothing.
“Staff suffer terribly because they feel like, ‘What good are the hospice experts if we can’t take care of patients’ pain?’” Periyakoil mentioned.
Often, the one factor they’ll do is stand again and respect the vets’ option to bear their ache, she mentioned.
Once, when Periyakoil was dressing the ulcer wounds of the affected person who refused “narc pills,” he started speaking in regards to the conflict. She didn’t press, simply saved working quietly on the injuries. As he stared on the ceiling, wincing, he confided in her a few time he was compelled to kill a pregnant teenager.
But this type of revelation is uncommon. With weeks or months left to stay, after a lifetime of silence about their most horrifying recollections, there usually isn’t sufficient time for vets to speak about them in any respect.
That’s one cause the VA has been attempting to start out end-of-life care earlier — to handle vets’ ethical misery or PTSD years earlier than they land in hospice, Widera mentioned.
Fleming’s medical doctors, for example, have urged him to contemplate psychological well being counseling or antidepressants. He refuses.
“I don’t want to take psychiatric drugs,” he mentioned. “The vets call them the happy pills. I don’t want any of those, because they change you. I don’t want to change.”
The emotional ache connects Fleming to his previous.
He was awarded 18 Air Medals for meritorious acts and heroism in flight. The loss and grief he skilled in Vietnam are woven into these recollections of victory and glory.
“You see all the combat. There’s a charge to it,” he mentioned. “And after a while, it bites you right in the ass. And once you’ve been bit, you’re bit for life. Nothing else works.”
This story is a part of a partnership that features KQED, NPR and Kaiser Health News, an editorially unbiased program of the Kaiser Family Foundation.
KHN’s protection of end-of-life and severe sickness points is supported partly by the Gordon and Betty Moore Foundation.
Related Topics Aging Mental Health Public Health End Of Life Hospice Opioids Palliative Care Veterans’ Health