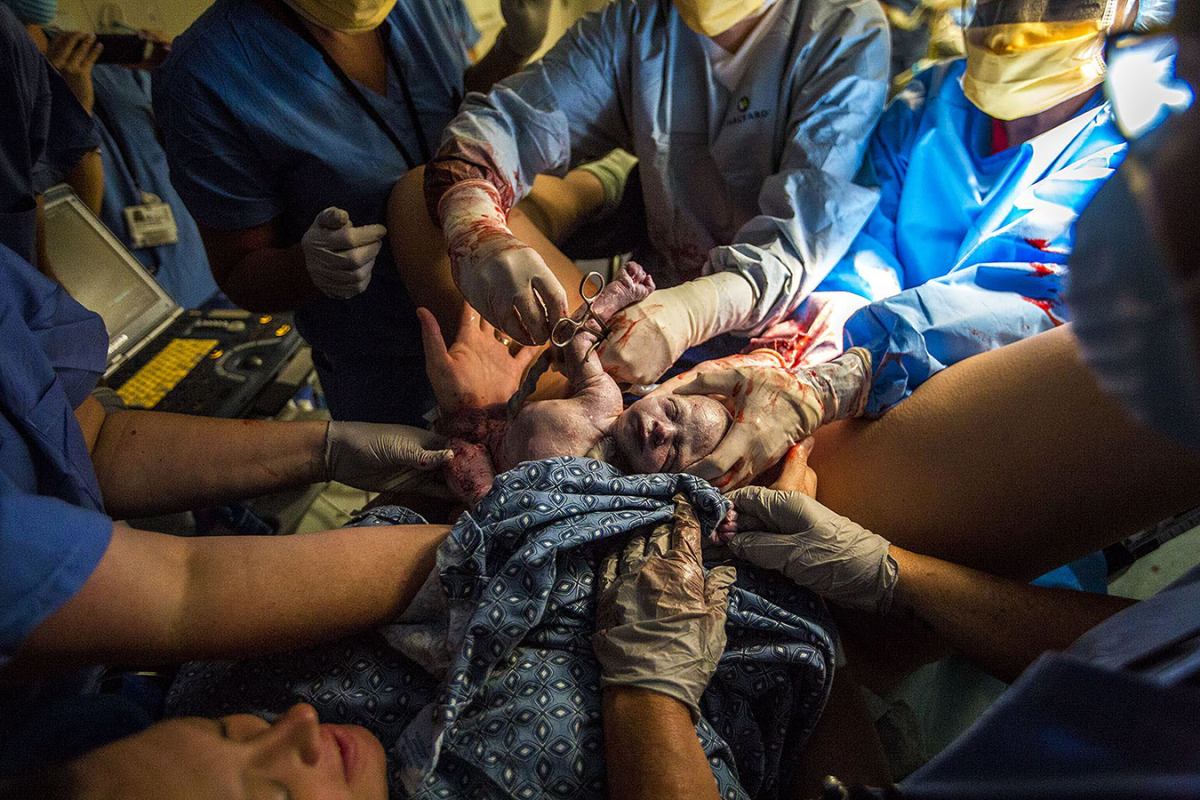
The tiny hand and forearm slipped out too early. Babies aren’t delivered shoulder first. Dr. Terri Marino, an obstetrician within the Boston space who focuses on high-risk deliveries, tucked it again contained in the boy’s mom.
“He was trying to shake my hand and I was like, ‘I’m not having this — put your hand back in there,’” Marino would say later, in spite of everything 5 kilos, 1 ounce of the newborn lay wailing underneath a heating lamp.
This is the story of how that child, Bryce McDougall, examined the perfect efforts of greater than a dozen medical staffers at South Shore Hospital in Weymouth, Mass., that day final summer season.
Bryce’s beginning additionally put to the check a brand new methodology of lowering cesarean sections developed at Dr. Atul Gawande’s Ariadne Labs, a “joint center for health systems innovation” at Brigham and Women’s Hospital and the Harvard T.H. Chan School of Public Health in Boston.
The story begins earlier than Bryce’s beginning, on the final day of August at about 9:30 within the morning.
Melisa McDougall has simply checked into South Shore, after a routine ultrasound. She’s in her 36th week, pregnant with twin boys. The medical doctors have warned Melisa that her placenta gained’t maintain out for much longer. She’s propped up in mattress, blond hair pulled right into a neat bun, make-up nonetheless contemporary, ordering a sandwich, when her common obstetrician arrives.
“How are you?” asks Dr. Ruth Levesque, sweeping into the room and clapping her palms. “You’re going to have some babies today! Are you excited?”
The first of the twins — Brady — is head-down, prepared for a traditional vaginal supply. But brother Bryce is horizontal on the high of Melisa’s uterus.
That’s one purpose Melisa is a candidate for a C-section. Babies don’t come out sideways. And there’s another excuse most medical doctors wouldn’t contemplate a vaginal supply in Melisa’s case, Levesque says. Four years in the past, she delivered the twins’ sister by cesarean.
“[Melisa] has a scar on her uterus,” Levesque explains, “so there’s a risk of uterine rupture — very rare, but there’s always a possibility.”
And that chance could also be larger for Melisa as a result of she’s 37 and having twins. But the McDougalls hope to have vaginal deliveries for each boys.
“I just feel like it’s better for the kids — better for the babies,” Melisa says.
Melisa McDougall hears comforting phrases from her nurse at South Shore Hospital in Weymouth, Mass. Part of the main target of the Team Birth Project is on facilitating communication amongst dad and mom, nurses and medical doctors.
How The ‘Team Birth Project’ Came To Be
Avoiding C-sections can be higher for a lot of mothers. With cesareans, there’s an extended restoration interval, a larger danger of an infection and an affiliation with harm and dying. And most C-sections aren’t medically obligatory, stated Dr. Neel Shah, who directs the Delivery Decisions Initiative at Ariadne Labs.
“We’re fairly confident that, when you look nationally, the plurality — if not the majority — of C-sections are probably avoidable,” stated Shah.
Those avoidable C-sections are the main target of the Team Birth Project, designed by Shah with enter from roughly 50 medical doctors, nurses, midwives, doulas, public well being specialists and client advocates who give attention to childbirth. South Shore Hospital is without doubt one of the pilot websites for the undertaking.
In describing the collaboration, Shah begins with an acknowledgement: Childbirth is sophisticated. You’ve acquired two sufferers — the mom and the newborn — and an advert hoc, usually shifting workforce that at a minimal consists of the mother, a nurse and a physician.
“So you’ve got three people who have to come together and become a very high-performing team in a really short period of time, for one of the most important moments in a person’s life,” Shah stated.
And this workforce has to carry out at its finest throughout an unpredictable occasion: labor.
Shah says medical doctors and nurses typically agree about three issues: when a mother is in lively labor; when a mother can positively strive for a vaginal supply; and when she will need to have a C-section.
“And then there’s this huge gray zone,” Shah stated. “And actually, everything about the Team Birth Project is about solving for the gray.”
To keep away from pointless C-sections when what to do isn’t clear, this hospital, along side Ariadne, has modified the way in which labor and supply is dealt with from begin to end.
First, girls aren’t admitted till they’re in lively labor. Secondly, the mother’s preferences — reminiscent of whether or not she’d like an epidural or not, whether or not she desires to have “skin-to-skin contact” with the newborn instantly after beginning — assist information the members of the labor workforce. The workforce members map the supply plan — together with mother’s preferences and the medical workforce’s steering — on a whiteboard, just like the one in Melisa’s room.
For the births of Bryce and Brady McDougall, the white erasable planning board will get a number of use.
Under “Team,” Levesque and registered nurse Patty Newbitt write their names. Melisa and Shaun McDougall are additionally listed as equal companions. The names of different members of the family or nurses could also be added and erased as labor progresses. Shah’s thought is that this workforce will “huddle” frequently all through the labor to debate the evolving beginning plan.
The beginning plan itself is split into three separate parts on the board: Maternal (the mother), Fetal (the newborn) and Progress (by way of how the labor is progressing). A mother with hypertension, as an example, may have particular consideration — and that will be famous on the board — however she might nonetheless have a standard labor and vaginal supply.
The whiteboard in Melisa McDougall’s hospital room particulars the beginning plan, together with her preferences and the medical workforce’s steering.
Good Communication Throughout Labor And Delivery Is Key
Dr. Kimberly Dever, who chairs the OB-GYN division at South Shore, highlights a bit of the whiteboard referred to as “Next Assessment.”
That class is included on the board, Dever stated, “because one of the things I often heard from patients is that they didn’t know what was going to happen next. Now they know.”
Asking the mother — and the couple — about their preferences for the supply is essential, too, Levesque stated.
“It forces us to stop and to think about everything with the patient,” she defined. “It makes us verbalize our thought process, which I think is good.”
Shaun McDougall walks throughout the room to get a more in-depth have a look at the whiteboard.
“Honestly, it seems like common sense,” he says. “I would always think the nurses would have something like this, but to have it out where mom and dad can see it — I think it’s pretty cool.”
With Melisa McDougall’s plan in place, everybody settles in, to attend. About 4 hours later, Melisa isn’t but feeling contractions. Levesque breaks the water sac round Brady.
“Looks nice and clear,” Levesque reviews. “Hey bud, come on and hang out with us,” she says to the newborn.
“So, you’re going to keep leaking fluid until you leak babies,” the physician explains to Melisa. “Whenever you start getting uncomfortable, we’ll get you an epidural at that point.”
Levesque strikes to the board and provides updates: Melisa is four centimeters dilated; her waters broke at 13:26; the subsequent evaluation can be after she will get an epidural.
The medical workforce insisted forward of time that Melisa comply with be numbed from the waist down if she desires to ship Bryce — the second twin — vaginally. Melisa agreed. The obstetricians could must rotate the newborn in her uterus, discover a foot and pull Bryce out, inflicting ache most ladies wouldn’t tolerate.
One of these medical doctors — Marino — peeks into the room and waves.
“Just came to say hi,” says Marino, who has extra expertise than most obstetricians in delivering infants positioned like Bryce. Along with Levesque, Marino has been seeing Melisa frequently via workplace visits.
Shaun McDougall asks the physicians in the event that they’ll pose for an image together with his spouse.
“Can we make funny faces?” asks Levesque.
“I want you to,” says Shaun. “You guys are like her favorite people on the planet.”
As the hours tick by, there’s a shift change, and registered nurse Barbara Fatemi joins the McDougall workforce. She checks Melisa’s ache stage frequently to find out when she’s prepared for the epidural.
Melisa says she isn’t feeling a lot, however provides that she has a excessive tolerance for ache. Shaun tells Fatemi he sees the pressure on his spouse’s face. Fatemi acts on Shaun’s evaluation, and calls an anesthesiologist to organize the epidural, one thing Shaun later says reinforces his feeling that they’re a workforce.
Levesque quickly arrives for the promised “next assessment.” Melisa is now 10 centimeters dilated and able to ship — however she should maintain on till nurses can get her into an working room.
The OR would be the proper place if the second child, Bryce, doesn’t shift his place, and the physician must do a last-minute cesarean.
“I’ll see you in a few minutes. No pushing without me, OK?” Levesque says over her shoulder as she heads to the OR to prep.
“I’ll try,” Melisa says, weakly. In a minute, nurses are rolling her down the corridor, following Levesque.
Almost 5 years in the past, two girls who had been wheeled into this hospital’s working rooms throughout childbirth died after present process C-sections. Though state investigators found no evidence of substandard care, Dever, the top of obstetrics, stated the hospital scrutinized the whole lot.
“When you have something like that happen, that expedites your efforts,” she stated. “Exponentially.”
Now, Dever stated, she sees a chance, via the Team Birth Project, to mannequin adjustments that might assist girls far and extensive.
“I would love women everywhere to be able to come in and have a safe birth and healthy baby,” she stated. “That’s why I’m doing it.”
‘They Did Not Flinch’
Dever is about to see her pilot examine of the Team Birth Project pushed to new limits by little Bryce McDougall. First, although, Melisa should ship Bryce’s twin brother, Brady. Even his beginning, the one which was anticipated to be simpler, is harder than anticipated.
Bent practically in half, her face beet pink, Melisa strains for 5 pushes. She throws up, then will get again to laboring. And abruptly, there he’s.
“Oh my goodness Brady, oh Brady,” wails Shaun. He follows a nurse holding his son over to a hotter.
Marino takes Shaun’s place subsequent to Levesque, who has reached inside Melisa to get the subsequent twin. Levesque’s mission is to seize Bryce’s toes and information him out. But the whole lot looks like fingers, not toes.
“That’s a hand,” she murmurs. “That’s a hand, too.”
Marino rolls an ultrasound throughout Melisa’s stomach, hoping the scan will present a foot. But Bryce’s toes are out of sight and out of attain.
Marino has had extra expertise than most obstetricians with transverse infants and this process, often called a breech extraction; she asks to strive. She reaches into Melisa’s uterus whereas Levesque strikes to Melisa’s proper facet and makes use of her forearm to shift Bryce and push him down. Dever has come into the room, and takes over the ultrasound. At least six medical doctors and nurses encircle Melisa, whose face is taut. Shaun frowns.
“Babe, you OK?” he asks.
Melisa nods. Bryce’s coronary heart charge is regular. But there’s nonetheless no signal of a foot. One little hand slips out and Marino nudges it again in.
“Open the table,” says Marino, her voice strained.
It’s open and prepared, her colleagues say, referring to the array of sterile surgical devices that Marino could quickly want, to start a C-section.
For 36 seconds, this room with greater than a dozen adults grows oddly quiet. Everyone is watching Marino twist her arm this fashion and that, decided to search out Bryce’s toes. Levesque leans arduous into Melisa’s stomach. Shaun bites his lip. Then Marino yanks at one thing — and her gloved hand emerges, clenching child Bryce by his two teeny legs.
“Oh babe, here he comes, here he comes — Woo!” squeals Shaun.
Shaun is overcome with emotion once more. Melisa manages an exhausted giggle. Baby Bryce retains everybody ready just a few extra seconds after which howls.
Levesque tends to Melisa, and Marino comes round to congratulate the brand new mother.
“He was fighting you, huh?” Melisa says, and laughs.
“I think I found at least five hands,” says Levesque.
Outside the OR, Levesque and Marino look relieved and elated. Both agree that almost all medical doctors would have delivered Bryce by C-section. But at South Shore, the McDougalls discovered a hospital that has challenged itself to carry out fewer C-sections, and a physician with expertise in these uncommon deliveries — one who knew and revered the dad and mom’ desire.
“They specifically wanted to have a vaginal delivery of both babies,” Marino says — and that was on her thoughts through the troublesome moments.
Bryce was high quality, says Marino, so the deciding issue for her was that Shaun and Melisa didn’t panic.
“They did not flinch — they were like, ‘Keep going,’” Marino remembers. “Sometimes the patient will say ‘stop,’ and then you have to stop.”
The infants’ father says he got here near requesting that, within the final minute earlier than Bryce was born.
“That part with the arm — it was pretty aggressive,” Shaun says.
But in that second, he provides, the sensation that he and Melisa had been a part of the workforce made a distinction.
“It made us more comfortable,” Shaun says, and that consolation translated to belief. “We trusted the decisions they were making.”
Melisa says she’s grateful for the vaginal supply.
“I did not want to have a natural birth and a C-section,” she says. “That would be a brutal recovery.”
Instead, 30 minutes after Bryce’s beginning, Melisa is nursing Brady and speaking with members of the family on FaceTime.
Next Assessment For The Team Birth Project
South Shore started utilizing the Team Birth method in April. Three different hospitals are additionally pilot websites: Saint Francis in Tulsa, Okla.; EvergreenHealth in Kirkland, Wash.; and Overlake in Redmond, Wash. The check interval runs for 2 years. In the primary 4 months at South Shore, the hospital’s major, low-risk C-section charge dropped from 31 p.c to 27 p.c — about 4 fewer C-sections every month.
Experts who contributed to the event of the Team Birth Project are wanting to see whether or not different hospitals can decrease their charges of C-section and maintain them down.
“Once you get past the early adopters, how do you demonstrate the benefits for others that aren’t willing to change?” requested Gene Declercq, a professor of group well being sciences at Boston University School of Public Health.
Declercq famous that a few insurers are starting to power that query, refusing to incorporate of their networks hospitals which have excessive C-section charges, or excessive charges of different pointless, if not dangerous, care.
The federal authorities has set a goal charge for hospitals: No greater than 23.9 p.c of first-time, low-risk moms needs to be delivered by C-section. The U.S. common in 2016 was 25.7 p.c.
The goal was put in place as a result of research has proven that if a lady’s first supply is a C-section, her subsequent deliveries are extremely prone to be C-sections, too — raising her (and her child’s) danger for problems and even dying.
Declercq stated the undertaking’s give attention to communication within the labor and supply room is sensible as a result of many physicians resolve when to carry out a cesarean based mostly on medical behavior or the tradition of their hospital.
“If you can impact that decision-making process, you can perhaps change the culture that might lead to unnecessary cesareans,” stated Declercq.
This story is a part of a reporting partnership with WBUR, NPR and Kaiser Health News.