This story additionally ran on NPR. This story will be republished totally free (details).
FORT SCOTT, Kan. — One Monday in February, 65-year-old Karen Endicott-Coyan gripped the wheel of her black 2014 Ford Taurus with each fingers as she made the hour-long drive from her farm close to Fort Scott to Chanute. With a uncommon type of a number of myeloma, she requires weekly chemotherapy injections to maintain the most cancers at bay.
About ‘No Mercy’
KHN’s year-long collection, No Mercy, follows how the closure of 1 beloved rural hospital disrupts a neighborhood’s well being care, financial system and equilibrium.
She made the journey in ache, having skipped her morphine for the day to have the ability to drive safely. Since she typically “gets the pukes” after therapy, she had her neighbor and pal Shirley Palmer, 76, come alongside to drive her again.
Continuity of care is essential for most cancers sufferers within the midst of therapy, which frequently requires frequent repeated outpatient visits. So when Mercy Hospital Fort Scott, the agricultural hospital in Endicott-Coyan’s hometown, was slated to shut its doorways on the finish of 2018, hospital officers had organized for its most cancers clinic — known as the “Unit of Hope” — to stay open.
Then “I got the email on Jan. 15,” stated Reta Baker, the hospital’s CEO. It knowledgeable her that Cancer Center of Kansas, the contractor that operated and staffed the unit, had determined to close it down too, simply two weeks later.
“There are too many changes in that town” to maintain the most cancers heart open, Yoosaf “Abe” Abraham, chief working officer of the Cancer Center of Kansas, later informed KHN. He added that sufferers can be “OK” as a result of they might get handled on the heart’s places of work in Chanute and Parsons.
From Fort Scott, these amenities are 50 and 63 miles away, respectively.
For Endicott-Coyan and dozens of different most cancers sufferers, the gap meant new challenges getting lifesaving therapy. “You have a flat tire, and there is nothing out here,” Endicott-Coyan stated, waving her arm towards the open sky and the pastures dotted with black Angus and white-faced Hereford cattle on both facet of the shoulderless, slender freeway she now should drive to get to her chemo appointment.
When the most cancers clinic at Mercy Hospital Fort Scott closed in January 2019, most cancers sufferers similar to Karen Endicott-Coyan needed to proceed their remedies in several areas. Endicott-Coyan has a uncommon type of a number of myeloma and now drives an hour from her farm close to Fort Scott, Kan., to Chanute, Kan., for weekly chemotherapy injections.(Christopher Smith for KHN)
Nationwide, more than 100 rural hospitals have closed since 2010. In every case, a novel however acquainted loss happens. Residents, after all, lose well being care providers as wards are shut and docs and nurses start to maneuver away.
But the ripple impact will be equally devastating. The financial vitality of a neighborhood takes a blow with out the hospital’s high-paying jobs and it turns into tougher for different industries to draw staff who need to reside in a city with a hospital. Whatever stays is vulnerable to withering with out the help of the stabilizing establishment.
The 7,800 residents of Fort Scott are reeling from the lack of their 132-year-old neighborhood hospital that was closed on the finish of December by Mercy, a St. Louis-based nonprofit well being system. Founded on the frontier within the 19th century and rebuilt right into a 69-bed fashionable facility in 2002, the hospital had outlived its use, with largely empty inpatient beds, the father or mother firm stated. For the subsequent yr, Kaiser Health News and NPR will observe how its residents fare after the closure within the hopes of answering urgent nationwide questions: Do residents in small communities like Fort Scott want a standard hospital for his or her well being wants? If not a hospital, what then?
Traveling The Distance For Cancer Care
Reta Baker, the hospital’s president who grew up on a farm south of Fort Scott, understood that the hospital’s closure was unavoidable. She scrambled to verify fundamental well being care wants can be met. Mercy agreed to maintain the constructing open and lights on till 2021. And Baker recruited a federally certified well being heart to take over 4 outpatient clinics, together with one contained in the hospital; former workers have been purchased out and proceed to function a rehabilitation heart; and the nonprofit Ascension Via Christi Hospital in Pittsburg reopened the emergency division in February.
As Fort Scott offers with the trauma of dropping a beloved establishment, deeper nationwide questions underlie the wrestle: Do small, rural communities want a standard hospital in any respect? And if not, how will they get the well being care they want?
But most cancers care in rural areas, which requires specialists and the acquisition and storage of a variety of oncology medicine, presents distinctive challenges.
Rural most cancers sufferers sometimes spend 66% more time touring every option to therapy than those that reside in additional city areas, in line with a latest nationwide survey by ASCO, the American Society of Clinical Oncology. Dr. Monica Bertagnolli, a cattle rancher’s daughter who’s now chair of ASCO’s board, known as this a “tremendous burden.” Cancer care, she defined, is “not just one visit and you’re done.”
ASCO used federal information to search out that whereas about 19% of Americans reside in rural areas, solely 7% of oncologists apply there.
People in rural America usually tend to die from most cancers than these within the nation’s metropolitan counties, in line with a Centers for Disease Control and Prevention report in 2017. It discovered 180 most cancers deaths per 100,000 folks a yr in rural counties, in contrast with 158 deaths per 100,000 in populous metropolitan counties.
Email Sign-Up
Subscribe to KHN’s free Morning Briefing.
The discrepancy is partly as a result of habits like smoking are extra frequent amongst rural residents, however the danger of dying goes past that, stated Jane Henley, a CDC epidemiologist and lead creator of the report. “We know geography can affect your risk factors, but we don’t expect it to affect mortality.”
From an workplace inside a former Mercy outpatient clinic, Fort Scott’s most cancers help group, Care to Share, continues its efforts to fulfill a few of the neighborhood’s wants — which in some methods have elevated because the Unit of Hope closed. It offers Ensure dietary dietary supplements, fuel vouchers and emotional help to most cancers sufferers.
Lavetta Simmons, one of many help group’s founders, stated she must elevate more cash to assist folks pay for fuel to allow them to drive farther to remedies. Last yr, on this impoverished nook of southeastern Kansas, Care to Share spent greater than $17,000 offering fuel cash to space residents who needed to journey to the Mercy hospital or farther away for care.
According to the U.S. Centers for Disease Control and Prevention, most cancers kills extra folks in rural America than within the nation’s metropolitan counties — 180 deaths per 100,000 folks in rural counties, in contrast with 158 deaths per 100,000 in extremely populated metropolitan counties.(Sarah Jane Tribble/KHN)
The group expects to spend extra on fuel this yr, having spent almost $6,000 through the first 4 months of 2019.
And the reserves of donated Ensure from Mercy are working out, so Simmons is reaching out to hospitals in close by counties for assist.
With Mercy Hospital Fort Scott closed, the probability of residents right here dying from their most cancers will develop, consultants fear, as a result of it’s that a lot tougher to entry specialists and coverings.
Krista Postai, who took over the Fort Scott hospital’s 4 major care clinics, stated it’s common for her employees to “see someone walk in [with] end-stage cancer that they put off because they didn’t have money, they didn’t have insurance, or it’s just the way you are. … We wait too long here.”
‘If They Can’t Cure Me, I’m Done’
Art Terry, 71, a farmer and Vietnam veteran, was one among them. Doctors found Terry’s most cancers after he broke a rib whereas bailing hay. When they discovered a mass beneath his armpit, it was already late-stage breast most cancers that had metastasized to his bones.
With his twice-weekly chemotherapy therapy out there within the “Unit of Hope,” Terry spent hours there along with his son and grandchildren telling tales and jokes as in the event that they have been in their very own front room. The nurses started to really feel like household, and Terry introduced them contemporary eggs from his farm.
“Dad couldn’t have better or more personalized care anywhere,” stated his son, Dwight, bleary-eyed after a manufacturing unit shift.
Art Terry, heart, stands for a household picture on the Mercy Hospital Fort Scott most cancers unit earlier than its January closure. From left are Terry’s daughter-in-law, Sabrina; granddaughters Aubry and Shaylee; son Dwight; and grandson Blaiton.(Courtesy of Dwight Terry)
Terry knew it was tough to search out reliable most cancers care. The scarcity of most cancers specialists in southeastern Kansas meant that many, together with Mercy Hospital Fort Scott’s sufferers, counted on touring oncologists to go to their communities a couple of times per week.
Wichita-based Cancer Center of Kansas has almost two dozen areas statewide. It started leasing house in Fort Scott’s hospital basement within the mid-2000s, the middle’s Abraham stated. The hospital supplied the employees whereas the Cancer Center of Kansas paid hire and despatched roving oncologists to drop in and deal with sufferers.
At its closing, the Unit of Hope served almost 200 sufferers, with about 40% of them on chemotherapy therapy.
When Art Terry was recognized, his son tried to speak to him about searching for therapy on the greater hospitals and educational facilities in Joplin, Mo., or the Kansas City space. The elder Terry wasn’t . “He’s like, ‘Nope,’” Dwight Terry recalled. “I’m going right there to Fort Scott. If they can’t cure me, I’m done. I’m not driving.’”
In the tip, because the elder Terry struggled to remain alive, Dwight Terry stated he would have pushed his father the hour to Chanute for therapy. Gas — already a mounting expense as they traveled the 20 miles from the farm close to tiny Prescott, Kan., to Fort Scott — can be much more pricey. And the journey can be taxing for his father, who traveled so little over the course of his life that he had visited Kansas City solely twice up to now 25 years.
As it turned out, the household by no means had to choose. Art Terry’s most cancers superior to his mind and killed him days earlier than the hospital’s most cancers unit closed.
What Happens Next?
As Endicott-Coyan and her pal Palmer drove to Chanute for therapy, they handed the time chatting about how the hospital’s closure is altering Fort Scott. “People started putting their houses up for sale,” Palmer stated.
Like many in Fort Scott, that they had each spent their days on the Fort Scott hospital. Endicott-Coyan labored in administration for greater than 23 years; Palmer volunteered with the auxiliary for six years.
Debbie Endicott, Karen Endicott-Coyan’s sister-in-law, drives to chemotherapy in Chanute, Kan. The journey takes an hour on largely slender, two-lane highways from Endicott-Coyan’s residence south of Fort Scott. “You can see there are no gas stations, there is nothing on the way,” Endicott-Coyan says. “There isn’t anything.”(Sarah Jane Tribble/KHN)
The hospital grew with the neighborhood. But because the city’s fortunes fell, it’s maybe no shock that the hospital couldn’t survive. But the intertwined historical past of Mercy and Fort Scott can be why its loss hit so many residents so exhausting.
Fort Scott started in 1842 when the U.S. authorities constructed a army fort to assist with the nation’s westward enlargement. Historians say Fort Scott was a boomtown within the years simply after the Civil War, with its recorded inhabitants rising to greater than 10,000 because the city competed with Kansas City to change into the biggest railroad heart west of the Mississippi. The hospital was an integral a part of the neighborhood after Sisters of Mercy nuns opened a 10-bed hospital in 1886 with a mission to serve the needy and poor. Baker, Mercy Hospital Fort Scott’s president, stated the most cancers heart was an extension of that mission.
The Unit of Hope started working out of the most recent hospital constructing’s basement, which was “pretty cramped,” Baker stated. As most cancers remedies improved, it grew so quickly that Mercy executives moved it to a spacious first-floor location that had beforehand been the enterprise places of work.
“Our whole purpose when we designed it was for it to be a place where somebody who was coming to have something unpleasant done could actually feel pampered and be in a nice environment,” Baker stated.
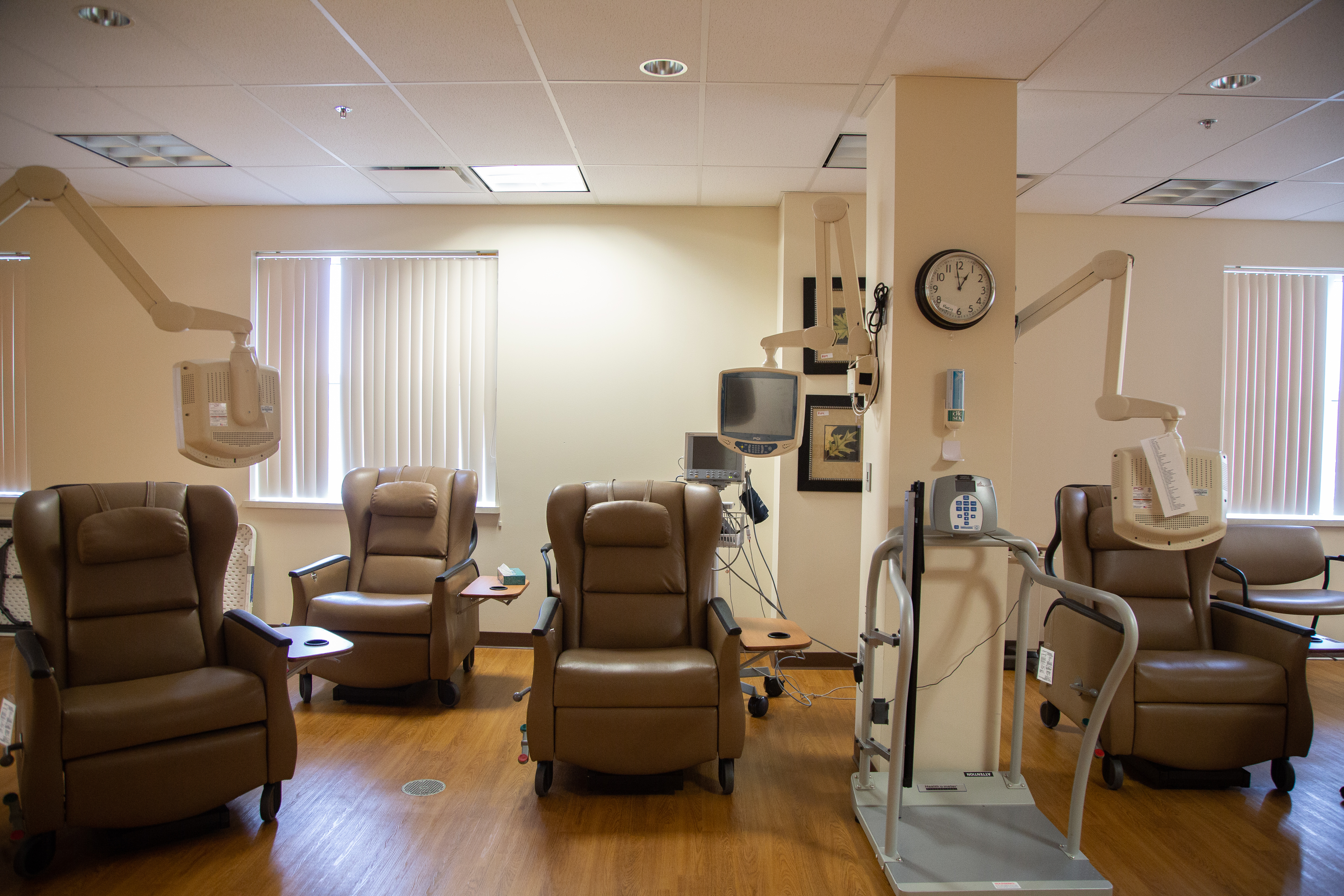
The heart, with its muted pure grays and browns, had home windows overlooking the entrance car parking zone and forested land past. Every affected person may look out the home windows or watch their private tv terminal, and every therapy chair had loads of house for members of the family to tug up chairs.
Endicott-Coyan and her husband, John Coyan, snicker whereas sitting of their kitchen. John, 74, started displaying indicators of dementia in 2015. Together, they run a cow-calf operation on 240 acres south of Fort Scott and go to church each Sunday. (Christopher Smith for KHN)
Endicott-Coyan labored for almost 24 years within the administration places of work at Mercy Hospital Fort Scott, specializing in reimbursement points. Diagnosed with most cancers in October 2015, Endicott-Coyan receives weekly chemo therapy and says she experiences a number of fatigue. “It’s 2019 and I’m still here and I’m still fighting,” she says. (Christopher Smith for KHN)
When Endicott-Coyan and Palmer arrived on the Cancer Center of Kansas clinic in Chanute in February, issues regarded starkly totally different. Patients entered a small room via a rusted again door. Three brown infusion chairs sat on both facet of the entry door and two tv screens have been mounted excessive on the partitions. A nurse checked Endicott-Coyan’s blood stress and ushered her again to a personal room to get a shot in her abdomen. She was prepared to go away about 15 minutes later.
The heart’s Abraham stated the Chanute facility is “good for patients for the time being” and never a “Taj Mahal” like Mercy’s Fort Scott hospital constructing, which he stated was too costly to take care of. Cancer Center of Kansas plans to open a clinic at a hospital in Girard, which is about 30 miles from Fort Scott, he stated.
Some oncology docs would say driving isn’t mandatory. Indeed, a couple of well being care methods throughout the nation, similar to Sanford Health in South Dakota and Thomas Jefferson University Hospitals in Pennsylvania, are administering some chemotherapy in sufferers’ houses. Oncologist Adam Binder, who practices at Thomas Jefferson in Philadelphia, stated “over 50% of chemotherapy would be safe to administer in the home setting if the right infrastructure existed.”
But the infrastructure — that’s, the nurses who would journey to deal with sufferers and a reimbursement mannequin to pay for such care inside our complicated well being care system — isn’t but in place.
Back within the automotive, Palmer took the wheel and Endicott-Coyan started planning for future most cancers remedies within the void left by Mercy Hospital Fort Scott’s closure. “I put a note on Facebook today and said, ‘OK, I have drivers for the rest of February; I need drivers for March!’”
This is the primary installment in KHN’s year-long collection, No Mercy, which follows how the closure of 1 beloved rural hospital disrupts a neighborhood’s well being care, financial system and equilibrium.
This story additionally ran on NPR. This story will be republished totally free (details).
Sarah Jane Tribble: [email protected]”>[email protected], @SJTribble
Related Topics Health Industry Cancer Hospitals Kansas No Mercy Rural Medicine src=”http://platform.twitter.com/widgets.js” charset=”utf-Eight”>