This story additionally ran on NPR. This story may be republished without cost (details).
For months, Sovereign Valentine had been feeling progressively run-down. The 50-year-old private coach, who goes by “Sov,” tried altering his exercise and food plan to no avail.
Finally, one Sunday, he drove himself to the hospital within the small city of Plains, Mont., the place his spouse, Jessica, occurred to be the doctor on name. “I couldn’t stop throwing up. I was just toxic.”
Do you’ve got an exorbitant or baffling medical invoice? Join the KHN and NPR’s Bill-of-the-Month Club and inform us about your expertise. We’ll characteristic a brand new one every month.
It turned out he was in kidney failure and wanted dialysis instantly.
“I was in shock, but I was so weak that I couldn’t even worry,” he mentioned. “I just turned it over to God.”
He was admitted to a close-by hospital that was outfitted to stabilize his situation and to get his first dialysis session. A social employee there organized for him to observe up with outpatient dialysis, thrice per week. She advised them Sov had two choices, each about 70 miles from his dwelling. They selected a Fresenius Kidney Care clinic in Missoula.
Just a few days after the remedies started, an insurance coverage case supervisor known as the Valentines warning them that since Fresenius was out-of-network, they could possibly be required to pay regardless of the insurer didn’t cowl. The supervisor added that there have been no in-network dialysis clinics in Montana, in response to Jessica’s handwritten notes from the dialog. (The insurance coverage firm disputes this, saying that its case supervisor advised Jessica there have been no in-network dialysis clinics in Missoula.)
Jessica repeatedly requested each the dialysis clinic workers and the insurer how a lot they may count on to be charged, however couldn’t get a solution.
Then the payments got here.
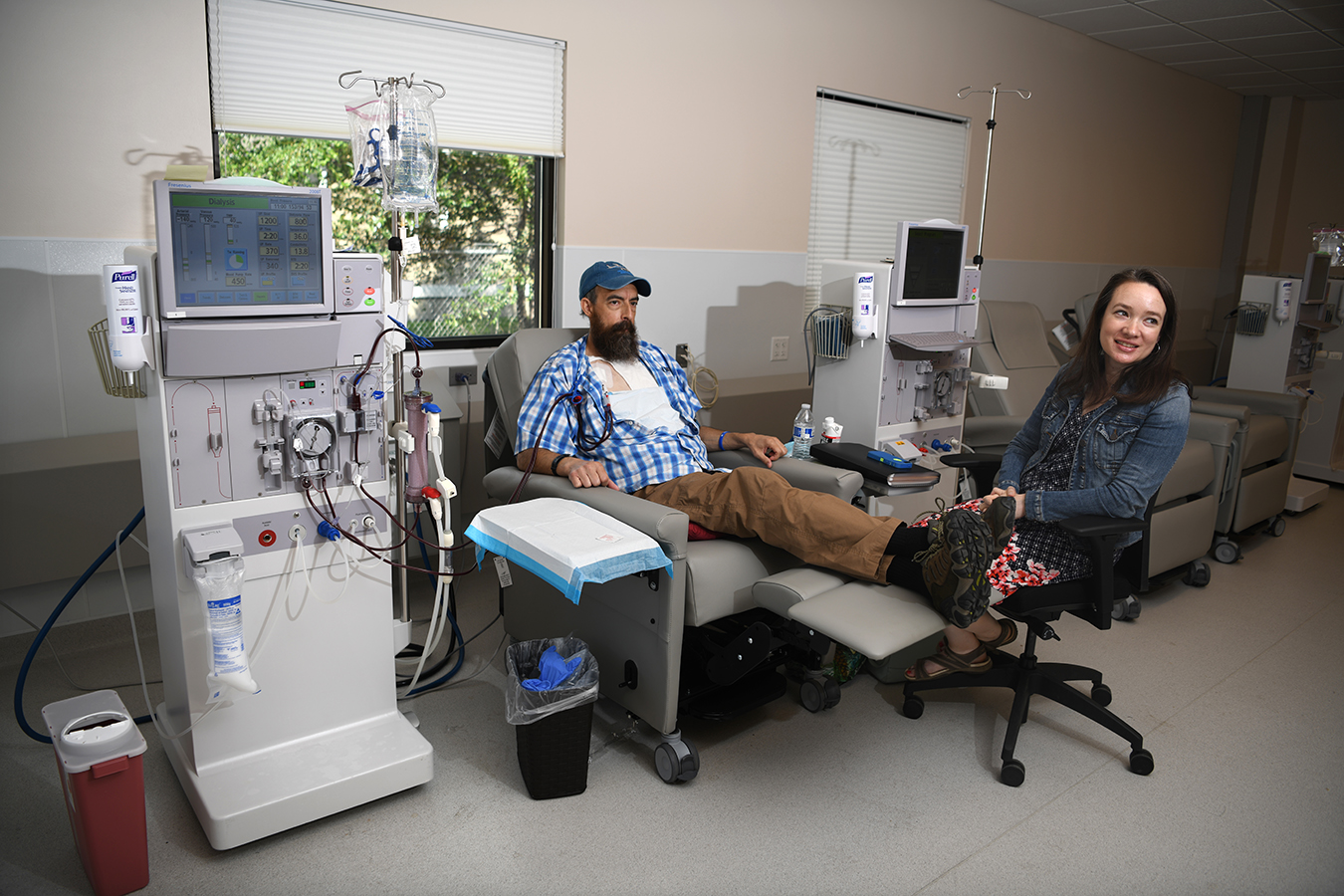
Valentine, a private coach in Plains, Mont., wants dialysis for his end-stage renal illness. When he first began dialysis remedies, Fresenius Kidney Care clinic in Missoula charged $13,867.74 per session, or about 59 occasions the $235 Medicare pays for a dialysis session.(Tommy Martino for KHN)
Patient: Sovereign Valentine, 50, a private coach in Plains, Mont. He is insured by Allegiance, by way of his spouse’s work as a health care provider in a rural hospital.
Total Bill: $540,841.90 for 14 weeks of dialysis care at an out-of-network Fresenius clinic. Valentine’s insurer paid $16,241.72. The clinic billed Valentine for the unpaid steadiness of $524,600.17.
Service Provider: Fresenius Medical Care, one in all two firms (together with rival DaVita) that management about 70% of the U.S. dialysis market.
Medical Treatment: Hemodialysis at an outpatient Fresenius clinic, three days per week for 14 weeks.
What Gives: As the dominant suppliers of dialysis care within the U.S., Fresenius and DaVita collectively type what well being economists name a “duopoly.” They can demand extraordinary costs for the lifesaving therapy they dispense — particularly when they don’t seem to be in a affected person’s community. A 1973 regulation permits all sufferers with end-stage renal illness like Sov to hitch Medicare, even when they’re youthful than 65 — however solely after a 90-day ready interval. During that point, sufferers are extraordinarily susceptible, medically and financially.
Fresenius billed the Valentines $524,600.17 — an quantity that’s greater than the standard cost of a kidney transplant. It’s additionally practically twice Jessica’s medical faculty debt. Fresenius charged the Valentines $13,867.74 per dialysis session, or about 59 occasions the $235 Medicare pays for a dialysis session.
When Jessica opened the primary invoice, she cried. “It was far worse than what I had imagined would be the worst-case scenario,” she mentioned.
Sov had a distinct response: “To me, it’s so outrageous that I just have to laugh.”
Dialysis facilities justify excessive expenses to commercially insured sufferers as a result of they are saying they make little or no cash on the charges paid for his or her Medicare sufferers, who — beneath the 1973 rule — make up the majority of their clientele. But practically $14,000 per session is extraordinary. Commercial payers often pay about 4 occasions the Medicare fee, in response to a recent study.
Dialysis firms are fairly worthwhile. Fresenius reported more than $2 billion in profits in 2018, with the overwhelming majority of its income coming from North America. The discrepancy in funds between Medicare and business payers provides dialysis facilities an incentive to deal with as many privately insured patients as attainable and to cost as a lot as they’ll earlier than dialysis sufferers enroll in Medicare. It may give dialysis facilities an incentive to cost the few out-of-network sufferers they see outlandish costs.
“The dialysis companies may think they can get closer to what they want from the health plans by staying out-of-network and charging these prices that are totally untethered to their actual costs,” mentioned Sabrina Corlette, a professor at Georgetown University’s Health Policy Institute. “They have the health plans over a barrel.”
Email Sign-Up
Subscribe to KHN’s free Morning Briefing.
One potential solution to save prices on dialysis is to change to a sort that may be finished at dwelling, which entails infusing fluid into the stomach. Called peritoneal dialysis, it’s common in Europe however comparatively uncommon within the U.S. In an govt order this month, President Donald Trump announced new incentives to extend uptake of these choices.
Brad Puffer, a spokesman for Fresenius Medical Care North America, mentioned the corporate is working with the Valentines “to immediately resolve the situation.”
“This person was unfortunately a victim of a health care system where insurers are increasingly shifting the financial burden to patients,” Puffer mentioned in a written statement Wednesday. “We are committed to doing the right thing so that our patients are not placed in the middle of these disputes.”
Resolution: As a doctor, Jessica Valentine is savvy about navigating the insurance coverage system. She knew it was vital to seek out an in-network supplier of dialysis. She and the insurance coverage firm case supervisor each searched on the insurer’s on-line supplier listing, she mentioned, and had been unable to seek out one. The drawback might have been looking for a “provider” moderately than a “facility” within the listing. Jessica ultimately wrote to the Montana insurance coverage commissioner to inquire if the dearth of a dialysis supplier violated a requirement that insurers preserve an “adequate network” of suppliers.
With assist from the state insurance coverage commissioner, she discovered that there was, in truth, an in-network dialysis clinic run by a nonprofit group that had not turned up in her insurer’s on-line search or the listing. She instantly organized for Sov to start out getting additional dialysis there. But the payments from Fresenius, in the meantime, had been including up.
After a reporter made inquiries, a monetary counselor at Fresenius advised Jessica that the Valentines certified for a reduction of 50%, primarily based on their revenue. That would nonetheless go away them a invoice of $262,400.08.
“It’s still a completely outrageous charge,” Jessica mentioned. “I want to pay what we owe and what’s reasonable and what his care actually cost.”
Unwilling to pay Fresenius extra, Allegiance mentioned Jessica ought to have discovered the in-network facility earlier. “There is always the potential for customers to misunderstand information about how their health plan works, especially in stressful situations,” a spokesman for Allegiance wrote.
Jessica is contemplating contacting a lawyer. If all else fails, the Valentines will contemplate submitting for chapter. A household physician who works at a rural hospital, Jessica now understands why a few of her sufferers keep away from testing and therapy for worry of the associated fee. “It’s very, very frustrating to be a patient, and it’s very disempowering to feel like you can’t make an informed choice because you can’t get the information you need.”
As a doctor, Jessica Valentine is savvy about navigating the insurance coverage system. She knew it was vital to seek out an in-network supplier for her husband’s dialysis. She and the insurance coverage firm case supervisor each searched on the insurer’s on-line supplier listing, she mentioned, and had been unable to seek out one.(Tommy Martino for KHN)
The Takeaway: Dialysis is a essential, lifesaving therapy. It will not be non-obligatory — irrespective of a affected person’s monetary scenario.
Insurers are obligated to have satisfactory networks for all coated medical companies of their plans, although “adequacy” is poorly outlined.
So, if it seems to be like there isn’t an in-network choice inside an inexpensive distance — for dialysis or extra primary companies from orthopedists or dermatologists — preserve digging. Keep in thoughts that dialysis clinics could also be listed as “facilities” moderately than “providers” in your listing.
If none can be found, search assist out of your state’s insurance coverage commissioner. Report your experiences — that’s a technique the commissioner can be taught that the names listed within the listing aren’t taking sufferers or are 50 miles away, for instance.
If you’ve got insurance coverage by way of an employer, you possibly can contact your advantages division to go to bat for you. If there isn’t a in-network choice, you need to get a dispensation to go out-of-network at in-network charges and with in-network copayments.
If you obtain a invoice for out-of-network care, don’t merely write the test. Ask for an itemized invoice and assessment the fees. You may also ask your insurance coverage firm to barter with the supplier in your behalf. See if the invoice counts as a “surprise bill” beneath your state’s regulation, during which case you could possibly be “held harmless” from extreme expenses.
And when all else fails, attempt to negotiate immediately with the supplier. They might need a monetary help coverage, or be keen to decrease the associated fee considerably to keep away from turning you over to a debt collector that may pay them pennies on the greenback.
NPR produced and edited the interview with Kaiser Health News’ Elisabeth Rosenthal for broadcast. Nick Mott of Montana Public Radio offered audio reporting.
Bill of the Month is a crowdsourced investigation by Kaiser Health News and NPR that dissects and explains medical payments. Do you’ve got an fascinating medical invoice you wish to share with us? Tell us about it!
This story additionally ran on NPR. This story may be republished without cost (details).
Jenny Gold: [email protected]”>[email protected], @JennyAGold
Related Topics Cost and Quality Health Care Costs Health Industry Multimedia States Bill Of The Month Montana src=”http://platform.twitter.com/widgets.js” charset=”utf-Eight”>