Mary Epp awoke from a deep sleep to the “high, shrill” sound of her dialysis machine’s alarm. Something was fallacious.
It was 1 a.m. and Epp, 89, was alone at dwelling in Marion Junction, Ala. No matter. Epp has been on dwelling dialysis since 2012, and she or he knew what to do: Check the machine, then name the 24/7 assist line at her dialysis supplier in Birmingham, Ala. to speak to a nurse.
The concern Epp recognized: Hours earlier than, a girl she employed to assist her out had put up two small baggage of dialysis answer as a substitute of the massive ones, and the answer had run out.
The nurse reassured Epp that she’d had sufficient dialysis. Epp tried to detach herself from the machine, however she couldn’t take away a cassette, a key half. A person on one other 24/7 assist line run by the machine’s producer helped with that downside.
Was it tough troubleshooting these points? “Not really: I’m used to it,” Epp stated, though she didn’t sleep soundly once more that night time.
If policymakers have their means, older adults with severe, irreversible kidney illness will more and more flip to dwelling dialysis. In July, the Trump administration made that clear in an executive order meant to essentially alter how sufferers with kidney illness are managed within the U.S.
Changing take care of the sickest sufferers — about 726,000 folks with end-stage kidney illness — is a prime precedence. Of these sufferers, 88% obtain therapy in dialysis facilities and 12% get dwelling dialysis.
By 2025, administration officers say, 80% of sufferers newly identified with end-stage kidney illness sufferers ought to obtain dwelling dialysis or kidney transplants. Older adults are certain to be affected: Half of the 125,000 individuals who study they’ve kidney failure annually are 65 or older.
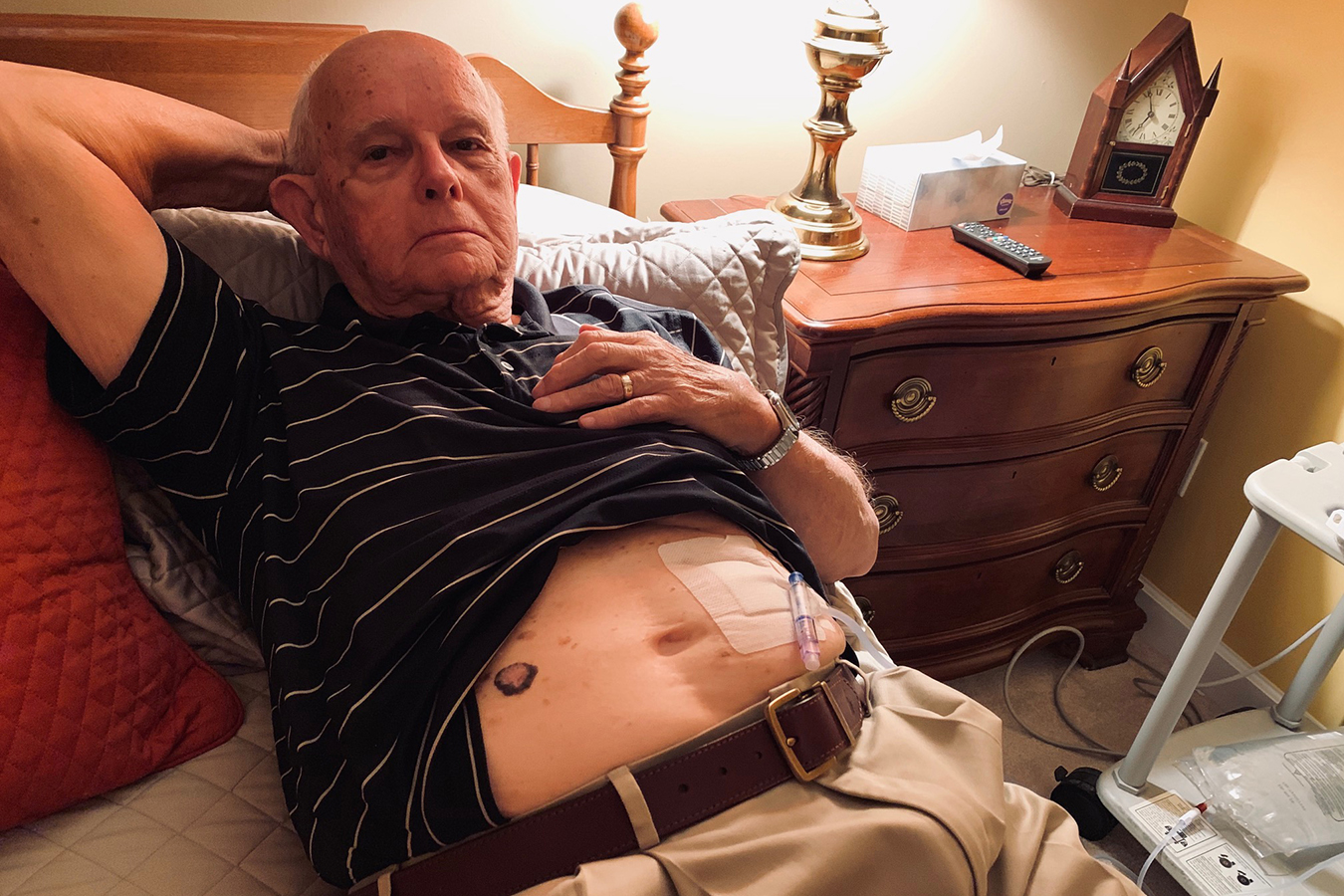
Mary Epp receives a telehealth seek the advice of from a group at a dialysis clinic in Birmingham, Ala., 90 miles away from her dwelling in Marion Junction. Epp does peritoneal dialysis at dwelling each night time whereas she sleeps.
Home dialysis has potential advantages: It’s extra handy than touring to a dialysis heart; restoration instances after therapy are shorter; remedy could be delivered extra usually and extra readily individualized, placing much less pressure on an individual’s physique; and “patients’ quality of life tends to be much better,” stated Dr. Frank Liu, director of dwelling hemodialysis on the Rogosin Institute in New York City.
But dwelling dialysis isn’t proper for everybody. Seniors with dangerous eyesight, poor fine-motor coordination, despair or cognitive impairment typically can’t undertake this remedy, specialists be aware. Similarly, frail older adults with a number of circumstances equivalent to diabetes, arthritis and heart problems might have important help from members of the family or pals.
The burden of offering this care shouldn’t be underestimated. In a current survey of caregivers providing complex care to members of the family, pals or neighbors, 64% recognized working dwelling dialysis gear as laborious — placing this on the prime of the record of adverse duties.
What experiences do older adults have with dwelling dialysis? Several seniors doing effectively on home-based therapies have been keen to debate this, however they’re a choose group. Up to a 3rd of sufferers who strive dwelling dialysis find yourself switching to dialysis facilities as a result of they undergo issues or lose motivation, amongst different causes.
It takes willpower. Jack Reynolds, 89, prides himself on being disciplined, which has helped him do peritoneal dialysis at dwelling in Dublin, Ohio, seven days per week for 3½ years.
With peritoneal dialysis, the remedy that Epp additionally will get, a fluid referred to as dialysate (a mixture of water, electrolytes and salts) is flushed right into a affected person’s stomach by a surgically implanted catheter. There, it absorbs waste merchandise and extra fluids over a number of hours earlier than being drained away. This kind of dialysis could be achieved with or with out a machine, a number of instances a day or at night time.
About 10% of sufferers on dialysis select peritoneal remedy, together with 18,500 older adults, in accordance with federal knowledge.
Reynolds prefers to manage peritoneal dialysis whereas he sleeps — a well-liked choice. His routine: After dinner, Reynolds units out two baggage of dialysate, ointments, sterile options, gauze bandages and a recent cassette for his dialysis machine with 4 tubes hooked up: two for the dialysate baggage, one for his catheter and one to expel dialysate on the finish.
Altogether, it takes him 23 minutes to collect every thing, clear the realm round his catheter and sterilize gear; it takes about as a lot time to take issues down within the morning. (Yes, he has timed it.) Just earlier than going to sleep, Reynolds hooks as much as his dialysis machine, which runs for 7.5 hours. (The quantity and frequency of remedy varies in accordance with a person’s wants.)
“I live a normal, productive life, and I’m determined to make this work,” Reynolds stated.
Jack Reynolds has been doing peritoneal dialysis at dwelling in Dublin, Ohio, seven days per week for the previous 3½ years. Each night time he makes use of two baggage of dialysate, ointments, sterile options, gauze bandages and a recent cassette for his dialysis machine with 4 tubes hooked up: two for the dialysate baggage, one for his catheter and one to expel dialysate able to be discarded.
It took 5 surgical procedures to efficiently implant a catheter on Reynolds’ left aspect due to scarring from earlier belly surgical procedures. He has needed to exchange three malfunctioning dialysis machines and discover ways to sleep on his proper aspect, so the tube related to his catheter isn’t compressed.
In the morning, his spouse, Norma, cleans the realm round his catheter, applies a gauze bandage and tapes an 18-inch extender hooked up to the catheter to his chest. He may do that himself, Reynolds stated, however “I wanted her to have some part in all this.”
Training is demanding. In December 2003, when Letisha Wadsworth began dwelling hemodialysis in Brooklyn, N.Y., she was working as an administrator at a social service company and needed to maintain her job. Doing dialysis within the night made that potential.
Home hemodialysis requires one to 2 months of schooling and coaching for each the affected person and, often, a care accomplice. With every therapy, two needles are caught into an entry level, often in a vein in a affected person’s arm. Through traces related to the needles, blood is pumped out of the affected person and thru a machine, the place it’s cleansed and waste merchandise are eliminated, earlier than being pumped again into the physique.
Only 2% of dialysis sufferers selected this feature in 2016, together with 2,800 older adults.
Letisha Wadsworth started dwelling hemodialysis 15 years in the past in an effort to maintain her job as a social service company administrator. Doing dialysis at her Brooklyn, N.Y., dwelling within the evenings made that potential.
The coaching was “rigorous” and “pretty scary for both of us,” stated Wadsworth, now 70, whose husband, Damon, accompanied her. “We learned a lot about dialysis, but we still didn’t know about issues that could arise when we got home.”
Issues that Wadsworth has needed to cope with: studying what to do if air received into one of many traces. Adjusting the speed at which her blood was pumped and flowed by the machine. And, not too long ago, getting a medical process to repair the entry website for her needles, which had clotted with blood.
Another concern: discovering area for 30 giant containers of provides (fluids, filters, needles, syringes and extra) that Wadsworth orders every month. They’re saved in two rooms in her home.
Over the years, Wadsworth has talked quite a bit to members of the family and pals about kidney failure and dialysis. “I wish I’d known about the relationship between blood pressure and kidney failure a lot earlier,” she stated. “I guess I thought all black people have high blood pressure: It just comes with the territory as opposed to what we can do to prevent it.” (High blood stress places folks prone to kidney failure.)
In 2013, Wadsworth had a stroke, which briefly paralyzed her left aspect. “I used to set up the [dialysis] machine, but now I use a walker and I can’t really stand and set everything up the way I used to.” Damon, 73, does this for her.
Wadsworth’s present routine: Dialysis begins round eight p.m. and goes for 5 hours, 4 days per week, in a devoted room in her home. She passes the time consuming dinner, watching TV, studying on her Kindle, speaking on the cellphone, visiting with pals or taking part in Scrabble with Damon.
Like most sufferers on dwelling dialysis, she will get blood checks as soon as a month and visits her nephrologist two weeks later to overview how she’s doing. A nurse, dietitian and social employee are additionally a part of her group on the Rogosin Institute.
Damon, a psychotherapist, admits it isn’t simple to stay his spouse with needles. “A lot of times, it hurts her, and it’s not fun for me to be the person doing that,” he stated. “But it’s just part of my life now. We’re thankful that home dialysis exists and we’re lucky enough to be able to do it.”
It could be overwhelming. Sharon Sanders, 76, thought she had the flu final yr when she had hassle respiration and retaining meals down. But when she landed within the hospital, docs informed her that her kidneys have been shutting down.
About half of the time, that is what occurs to individuals who find yourself on dialysis: They study out of the blue that their kidneys aren’t working reliably anymore.
Like many individuals, Sanders was shocked. After going to lessons and speaking to a niece who’s a registered nurse, she selected peritoneal dialysis. “I liked that I can do it at home, by myself, and I don’t have to stick myself with needles,” she stated.
Training took a couple of week at a clinic in Mesa, Ariz. “It came very easy for me,” stated Sanders, who lives in Gold Canyon, Ariz., and who started her nightly routine of six hours of peritoneal dialysis, 5 days per week, final August.
She doesn’t pay something for the remedy, which is roofed for her by Medicare and Tricare insurance coverage, a profit Sanders has due to her husband’s army service. (He died in 2017). Medicare Part B pays 80% of the price of dialysis at dwelling, and supplemental protection (together with, as an illustration, a Medigap coverage, a retiree coverage from an employer or Medicaid) typically picks up the rest.
Sanders is a frequent customer to Home Dialyzors United Facebook support group and one other website, Home Dialysis Central. Another website, My Dialysis Choice, is a helpful useful resource for folks deciding whether or not dwelling dialysis is correct for them.
Even although Sanders, who has arthritis of the backbone, doesn’t discover her dialysis routine particularly burdensome, she typically will get overwhelmed. “I don’t have any energy too much of the time,” she stated. “I find myself thinking, What’s my purpose for doing this? Is it worth it if we’re all going to die anyway?’”
Finding wanted assist. Until final November, when her husband of 68 years died, Mary Epp relied on him to get her prepared for peritoneal dialysis, which she receives each night time whereas she sleeps for 9 hours.
Now, an aide is available in a 7 p.m. to assist Epp take a shower and set issues up earlier than dialysis begins an hour later. Another girl is available in at 5 a.m. to take her off dialysis, clear every thing up and repair her breakfast.
“I’ve gotten a lot more feeble than I was” when dwelling dialysis started in 2012, stated Epp, who admitted she was “terrified” when a doctor identified her with kidney failure.
But the advantages of dwelling remedy, which is overseen by a group at a dialysis clinic 90 miles away in Birmingham, stay value it, she stated. “You just go to bed and wake up the next morning and you’re ready to go and meet the day.”