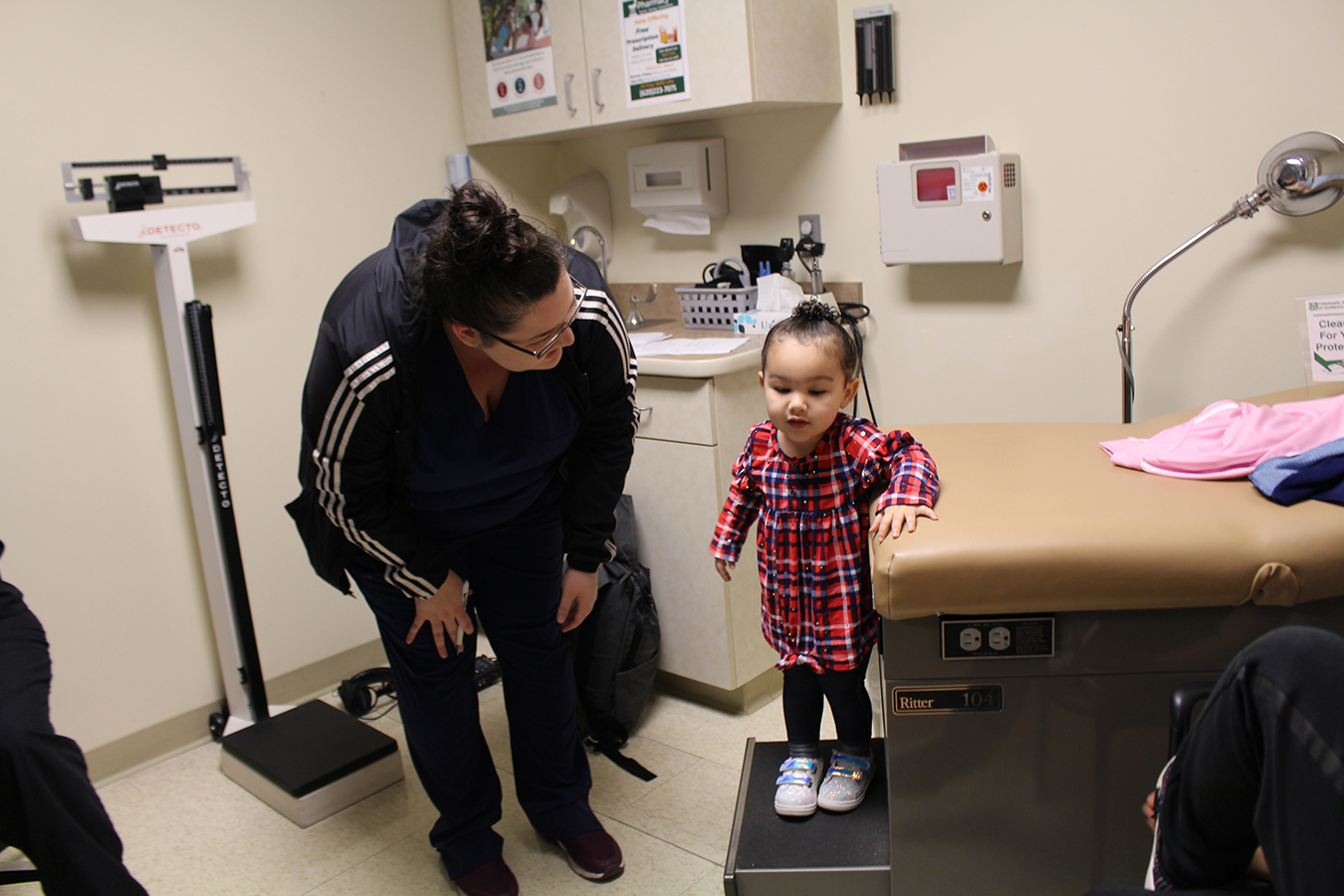
Eliza Oliver helps her daughter, Taelyn, step down from the examination desk after her wellness examine at Community Health Center. The youngster’s physician, who labored on the now-closed hospital, has been given a medical scribe who takes notes. The go to this time appeared extra “personal,” Oliver says.
This story additionally ran on NPR. This story could be republished at no cost (details). FORT SCOTT, Kan. ― Dr. Max Self grabbed a sanitary wipe and cleaned off the small flashlight in his fingers. More than 20 years as a household physician in rural Fort Scott, Kan., has taught him a number of methods: “I’ve got my flashlight. See? Look, you want to hold it?”
Two-year-old Taelyn’s brown eyes develop spherical and her tiny hand reaches out. But, first, Self makes certain she opens her mouth extensive and he friends down. Behind him sits one other workers member ― a medical scribe. Self’s scribe provides him the flexibility to “focus on people,” reasonably than toggling between a pc display and the affected person. It’s a brand new perk he didn’t have when he labored at Mercy Hospital.
That beloved hospital closed one 12 months in the past and, within the passing months, the small city’s anger and concern developed into grief, nervousness and ― these days ― pragmatic hope. Most of the handful of physicians on the town stayed, taking jobs at a regional federally certified well being care heart that took over a lot of the clinic work from Mercy. The emergency division, after closing for 18 days, was reopened quickly ― run by a hospital 30 miles south.
It’s not “all gloom and doom, although we all wish we had a hospital ― no doubt about it,” insurance coverage agent Don Doherty mentioned through the city’s weekly Chamber of Commerce espresso on Dec. 12.
Nationwide, demise charges have been greater in rural America in contrast with city areas for the reason that 1980s, and the hole continues to widen. More rural residents dwell with power circumstances, like diabetes, that have an effect on their each day lives, and there’s a greater proportion of older residents. Rates of smoking and untimely births are comparatively excessive, and folks usually die youthful right here than the nationwide common.
Since 2010, 120 rural hospitals have closed throughout the nation ― 19 on this 12 months alone, based on knowledge from the University of North Carolina’s Cecil G. Sheps Center for Health Services Research. A national analysis of Medicare price studies discovered that 21% of the nation’s remaining rural hospitals are at excessive threat of closing.
“Frankly, it’s not getting better,” mentioned Dr. Daniel DeBehnke, examine co-author and a managing director with Navigant’s well being care follow.
A 12 months in the past, after Mercy gave a 90-day discover that it might shut, City Manager Dave Martin mentioned the betrayal felt by metropolis leaders led to legal professionals and calls with different well being care programs about taking on the ability. Now, Martin has realized “we will not have ― or do we need ― a hospital.”
But, if not a hospital to take care of rural communities like Fort Scott with its 7,800 residents, what is required? The solutions to that query play out day-after-day right here and will maintain classes for the remainder of the nation.
For months after Mercy Fort Scott Hospital closed, sufferers couldn’t get appointments with Dr. Max Self rapidly. “I don’t like to hear that,” Self says. His new employer, Community Health Center of Southeast Kansas, assigned him a medical scribe, who does his laptop work. Now, Self says, he can see extra sufferers.
‘You Will Be Taken Care Of’
Self has cared for his share of struggling sufferers on this city, the place 1 in four kids dwell in poverty, and its most important hall ― U.S. 69 ― is lined with fast-food eating places. But Fort Scott is “not far off” from what it must be wholesome. Sure, residents must journey south 30 miles to Pittsburg, Kan., or north 90 miles to the Kansas City, Kan., space to be hospitalized, however “you will be taken care of,” he mentioned.
Self’s new employer is Community Health Center of Southeast Kansas, which as a federally certified well being heart will get the next stage of presidency reimbursement for Medicare and Medicaid sufferers than Mercy did, mentioned Jason Wesco, government vice chairman at CHC.
The heart also can acquire grants to handle the uninsured, which is essential in states like Kansas that didn’t broaden Medicaid, although Wesco mentioned it has not acquired any for Fort Scott.
Wesco estimates 90-95% of the well being care supplied earlier than the hospital closed continues to be out there domestically. And providers have been added, together with a much-needed therapist on-site for behavioral well being and telehealth entry to a psychiatrist and substance abuse providers.
“Drive up there, go into the parking lot, you’re like ‘There’s a lot of people here,’” Wesco mentioned. CHC’s Fort Scott amenities have crammed extra prescriptions and carried out extra mammograms in a month than the hospital “ever did,” he mentioned.
Jason Wesco, government vice chairman of Community Health Center, says he believes “the best people in the world” are from southeastern Kansas, the place the federally certified well being heart he helps run is predicated. Since the middle took over clinics in Fort Scott, Wesco says, the first care providers they supply can “lift up this place. … We can fix it, we just need time.” (Sarah Jane Tribble/KHN)
Community Health Center’s Fort Scott amenities have crammed extra prescriptions and carried out extra mammograms in a month than the hospital “ever did,” Wesco says.(Sarah Jane Tribble/KHN)
Local residents like 28-year-old Eliza Oliver, whose daughter, Taelyn, simply handed her annual wellness examine with Dr. Self, mentioned it’s a lot cheaper to get care and prescriptions on the new well being heart. That half is nice, Oliver mentioned, however she nonetheless worries about the way forward for emergency care on the town and the place folks can ship infants.
Another Catholic hospital chain, Ascension Via Christi, which has a facility 30 miles away in Pittsburg, Kan., stepped in on the final minute to function Mercy’s previous emergency room, signing a two-year settlement. This was very important: While a lot of the remainder of Mercy Hospital Fort Scott had been underused and affected person rooms sat empty, the ER dealt with almost 9,000 folks the 12 months earlier than it closed.
Mercy Hospital delivered greater than 230 infants between July 2017 and June 2018. A number of months in the past ― after the hospital closed ― Oliver drove a buddy who was in labor throughout the Missouri border greater than 20 miles to ship. “We had to jet over there and even though we made it in time, it’s nerve-wracking,” Oliver mentioned.
Another Catholic hospital chain, Ascension Via Christi, stepped in on the final minute to function Mercy’s previous emergency room, signing a two-year settlement.
Not having a group hospital does require a brand new mindset. The group nonetheless has an obstetrician, however docs ship sufferers out of city to have their infants. By June this 12 months, Ascension’s Fort Scott ER workers had delivered three infants for expectant moms who didn’t go away sufficient time.
Randy Cason, president at Ascension’s Pittsburg hospital, drove to Fort Scott to inform the weekly chamber espresso that docs wanted to “counsel and educate” moms that it’s now not a 10-minute drive to the hospital.
Sherise Beckham, a former Mercy dietitian, was anxious on mattress relaxation this spring whereas awaiting a child. “You’re on a two-lane highway; a lot of times you get behind a semi, behind a tractor,” Beckham laughed. “Sometimes, you are lucky if you have cell service.”
Beckham’s supply didn’t go as deliberate. After driving to Ascension’s Pittsburg hospital to satisfy her household physician, she had an surprising cesarean part, and the child, whose coronary heart fee dropped dramatically, was transferred to a neonatal intensive care unit an hour away from dwelling in Joplin, Mo. Now, eight months later, the child is wholesome although he continues to see a bodily therapist who screens his developmental progress.
Dietitian Sherise Beckham cooks dinner along with her household — husband Tanner, Eight-month-old Barrett and 2-year-old Warren.
Recent research by Katy Backes Kozhimannil, an affiliate professor on the University of Minnesota School of Public Health discovered that rural residents have a 9% higher probability of dying or struggling issues corresponding to coronary heart failure, stroke and the necessity for blood transfusions throughout childbirth in contrast with non-rural residents.
Federal policymakers have mentioned they need to do higher. President Donald Trump’s administration this 12 months set new Medicare cost insurance policies that included extra telehealth providers and altered some funds for rural hospitals. Seema Verma, the administrator for the Centers for Medicare & Medicaid Services, additionally promised a brand new rural well being cost mannequin and “a lot of people are waiting with bated breath,” mentioned George Pink, a senior analysis fellow at UNC’s Sheps Center.
CMS declined to touch upon the timing of the proposal.
Congress, too, has made overtures to passing laws. Maggie Elehwany, lead federal lobbyist for the National Rural Health Association, mentioned the Affordable Care Act’s promise that hospitals would have extra insured sufferers and fewer unhealthy debt “never really unfolded in rural America.” The 14 states which have not adopted Medicaid expansion are largely rural and plenty of are within the South, the place the best variety of hospitals have closed.
Sisters of Mercy nuns based the Fort Scott hospital in 1886. A mantra etched in stone over the doorway of 1 previous Mercy hospital constructing learn: “Dedicated to suffering humanity.”
Signs Of Change
Catholic nuns based the Fort Scott hospital greater than a century in the past and 89-year-old Fred Campbell nonetheless remembers a mantra etched in stone over the doorway of 1 previous Mercy hospital constructing: “Dedicated to suffering humanity.”
“We always felt that, man, come hell or high water, you’re gonna be with us and you’re not going to abandon us,” Campbell mentioned.
But precisely a 12 months in the past, its then-owner, St. Louis-based Mercy, a serious well being care conglomerate with greater than 40 hospitals, declared it now not financially viable.
Within weeks of Mercy closing, a newly constructed $9 million grocery retailer closed. A number of weeks later, the most cancers heart closed and, by October, the city’s dialysis heart had closed, too. John Leatherman, professor for the division of agricultural economics at Kansas State University, mentioned there’s little doubt Bourbon County took “a big hit” when the hospital was shuttered.
Roxine Poznich misplaced her revenue when her job at Mercy ended. After greater than 20 years on the hospital, the 73-year-old mentioned she now finds herself paying for groceries along with her bank card ― despite the fact that she is uncertain whether or not she will be able to pay the invoice on the finish of the month. “I’m scared,” Poznich mentioned.
Roxine Poznich, proprietor of Books & Grannies in Fort Scott, Kan., was a 27-year worker of Mercy Hospital in Fort Scott. She misplaced her job when the hospital closed and now manages her bookstore full time.
But Fort Scott financial improvement director Rachel Pruitt mentioned the lack of the hospital has not affected town’s gross sales tax income. Manufacturers just like the group’s largest employer, Peerless Architectural Windows and Doors, with its 400 jobs, proceed to broaden ― simply down the highway from the place Mercy’s 177,000-square-foot hospital constructing nonetheless stands.
City leaders say ideally the group would “right-size” its well being care. That would come with protecting the present outpatient clinics that present major care and an emergency division but additionally including some inpatient beds, permitting residents with short-term hospitalization to remain native. Pruitt mentioned there has even been speak of including a wound heart that might deal with accidents among the many city’s industrial employees.
And, although the principally empty Mercy Hospital constructing appears like a white elephant, that too could quickly change: Mercy lately introduced it might donate land in a repurposed nook of its property to Community Health Center. Health heart leaders have employed an architect for a brand new constructing that may most likely be about 30,000 sq. toes. Wellness, imaging, walk-in care, a ladies’s well being heart, dental care and expanded major and specialty care can be out there.
Fort Scott City Manager Dave Martin says he is aware of the city won’t ever have one other full-service hospital, and it doesn’t want one. Instead, Martin and his workers consider they want “right-sized” well being care. (Christopher Smith for KHN)
Reta Baker was the president of Mercy Hospital Fort Scott when it closed. She has since offered her home and moved nearer to her new job at CHC headquarters in Pittsburg, Kan.(Sarah Jane Tribble/KHN)
ER operator Ascension declined requests for interviews, however spokeswoman Michelle Kennedy mentioned the Pittsburg management group is “working on plans related to our presence in Fort Scott in the near future” however couldn’t launch particulars. City leaders say they’re assured an ER will stay.
In the background, there may be Reta Baker. Residents right here denounced the previous president of Mercy Hospital Fort Scott on the time of the closure. She offered her home and moved nearer to her new job with CHC, at its headquarters in Pittsburg, Kan.
Baker, who began her profession as a nurse at Fort Scott’s hospital in 1981 and grew up close by, mentioned she continues to “be engaged in a lot of conversations” in regards to the group’s future. The subsequent 12 months may have rising pains, she mentioned, however she believes the well being care wanted for residents is there.
“Now, we need to cement it,” she mentioned.
This is the fifth installment in KHN’s year-long sequence, No Mercy, which follows how the closure of 1 beloved rural hospital disrupts a group’s well being care, economic system and equilibrium. Coming in 2020, a podcast from KHN with extra voices and tales from Fort Scott, Kansas.