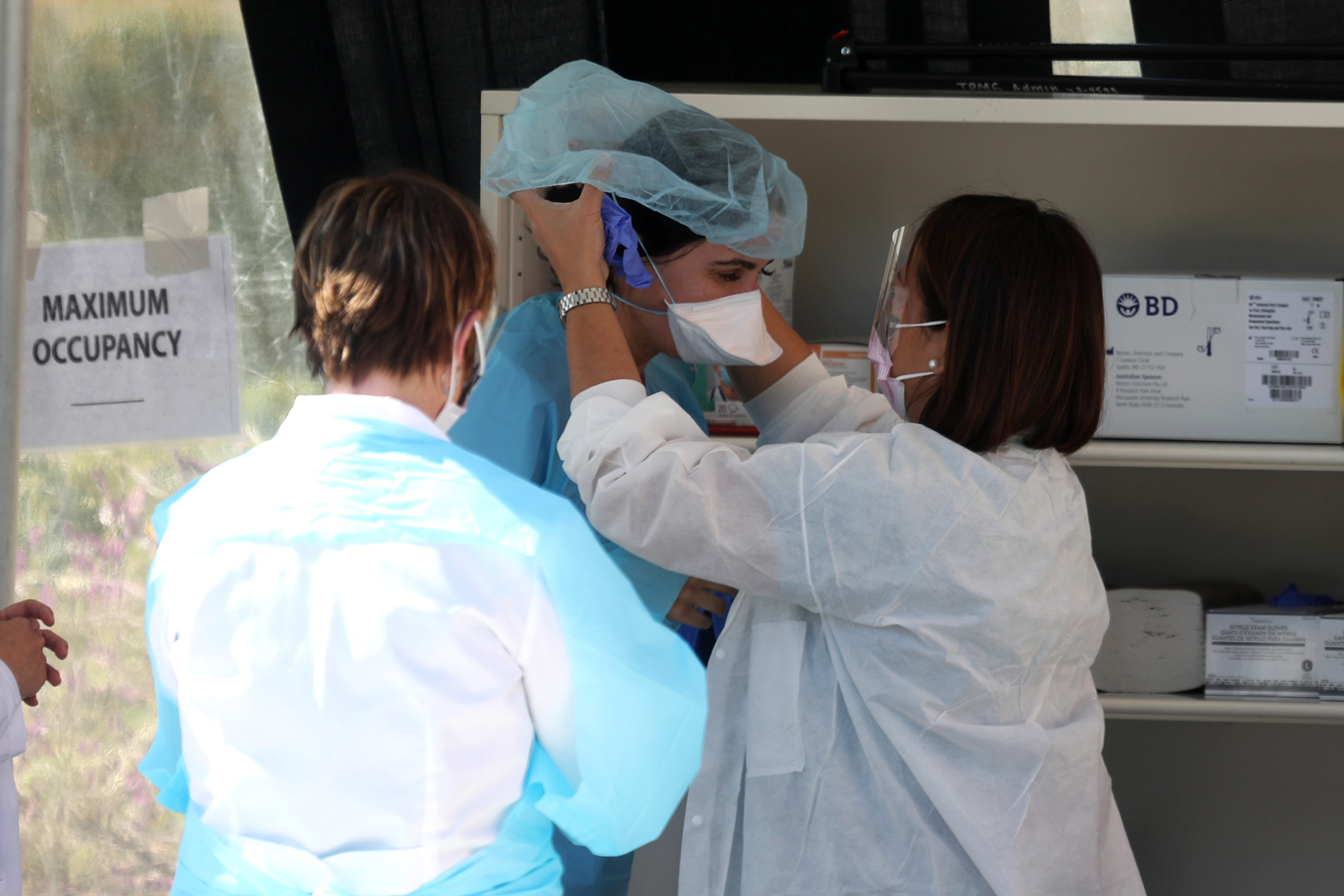
On Tuesday, Dr. Jeanne Noble devoted time between affected person visits to hanging clear 2-gallon plastic luggage at every of her colleagues’ workstations. Noble is a professor of emergency medication and director of the UC-San Francisco medical middle response to the novel coronavirus that has permeated California and reached into each U.S. state.
The luggage have been there to carry private protecting tools — the masks, face shields, robes and different gadgets that well being care suppliers depend on day by day to guard themselves from the viruses shed by sufferers, largely via coughs and sneezes. In regular instances, security protocols would require these things be disposed of after one use. But simply weeks into the COVID-19 pandemic, provides of protecting gear at UCSF are already so low that medical doctors and nurses are wiping down and reusing virtually every part besides gloves.
“It is not a foolproof strategy at all; we all realize the risk we are taking,” Noble stated. But as provides dwindle, she more and more finds herself asking the parents answerable for an infection management on the hospital if they’ll make adjustments to protocols. “As days go by, one regulation after the other goes out,” she stated.
Noble is among the many Bay Area physicians applauding the choice this week by seven Bay Area counties and a number of others throughout California to order residents to shelter in place for the foreseeable future, directives which are upending life for tens of millions of individuals and shuttering colleges and companies throughout the state. Without swift and dramatic adjustments to curb transmission of the virus, hospital officers say, it’s only a matter of time earlier than their well being methods are overwhelmed.
Interviews with California physicians on the entrance strains of COVID-19 provide a sobering portrait of a well being care system getting ready for the worst of a pandemic that might be months from peaking. In the Bay Area, the battle is being waged hospital by hospital, with extensive variations in assets.
The tent the place Noble tended to sufferers this week was set as much as take care of a latest rise in folks exhibiting up with respiratory sickness. Even with out the coronavirus risk, UCSF’s emergency room is a busy one, and medical doctors regularly see sufferers in hallways and different areas. But the present outbreak makes that shut contact unsafe. So as an alternative, everybody who involves the hospital is being triaged. Most folks with fever, cough or shortness of breath are diverted to the tent, which is heated and has damaging air stress to forestall the unfold of an infection. For now, the tempo is manageable, however Noble fears what’s forward.
Farther south, in Palo Alto, Stanford Medical Center was testing sufferers with respiratory issues in its parking storage. The personal college hospital has extra protecting gear than the general public one in San Francisco; a worldwide scavenger hunt a number of weeks in the past bolstered provides, although Stanford, too, has tailored protocols to be extra sparing with some gadgets.
“We don’t have an unlimited supply,” stated Dr. Andra Blomkalns, professor and chair of the Stanford School of Medicine’s Department of Emergency Medicine. “But at least we’re not looking at our last box.”
The whole nation is brief on protecting gear, a results of each the surging demand for such tools because the virus spreads and the implosion of provide chains from China, the place a lot of the tools is manufactured.
Noble believes some tools will should be made domestically. “If the [federal] government doesn’t step in and force manufacturing of these products here now, we are going to run out,” she stated.
Empty provide closets have an effect on everybody who wants care, together with coronary heart assault victims and folks in want of emergency surgical procedure, stated Dr. Vivian Reyes, president of the California chapter of the American College of Emergency Physicians and a working towards emergency doctor within the Bay Area.
“I know it’s really hard for us Americans because we’re never told no,” she stated of the shortfall of provides. “But we’re not in normal times right now.”
And protecting tools isn’t the one factor in brief provide.
Until a couple of days in the past, UCSF needed to depend on the San Francisco Department of Public Health for coronavirus testing, and a scarcity of check kits meant clinicians may check solely essentially the most critically unwell. The scenario improved March 9, when the college began operating checks created in its personal lab. First, there have been 40 checks a day. By Tuesday, there have been 60 to 80. But a brand new scarcity looms: The hospital has simply 500 testing swabs left.
Stanford pathologist Benjamin Pinsky constructed an in-house check that has been authorized to be used by the federal Food and Drug Administration. Since March three, Stanford has used it to check greater than 500 sufferers, 12% of whom had examined constructive as of Tuesday. The college has been operating checks for different hospitals as nicely, together with UCSF. It’s a dramatic enchancment from a couple of weeks in the past, when Stanford relied on its county lab.
Blomkalns noticed a sick affected person in mid-February, earlier than the hospital had its personal check kits, who had signs of COVID-19 however didn’t qualify for testing underneath the slender federal pointers in place on the time. He went residence, solely to return to the hospital after his situation deteriorated. This time, he was examined and it got here again constructive.
In Santa Clara County, residence to Stanford, 175 folks have examined constructive for COVID-19 and 6 have died. Late final week, the medical middle’s emergency division noticed the very best variety of sufferers in sooner or later in its historical past. Blomkalns doubts it’s as a result of there are extra circumstances in her space. “If you don’t test, you don’t have any cases,” she stated.
Blomkalns worries about staffing shortages as well being care employees are inevitably uncovered to the virus. As of Tuesday, one physician within the Stanford ER had examined constructive. At UCSF, six well being care suppliers had.
Not all Bay Area hospitals are seeing a flood of sufferers. In reality, some have fewer sufferers than traditional, as they’ve canceled elective surgical procedures in anticipation of a COVID-19 surge.
The medical doctors treating COVID-19 sufferers say almost all who check constructive have a cough. They complain of fatigue, physique aches, complications, runny noses and sore throats. While most individuals are nicely sufficient to get well at residence, those that get critically unwell have a tendency to take action of their second week of signs, and may deteriorate in a short time, a number of medical doctors famous. “We are recommending that patients get intubated a little earlier than they might otherwise,” stated Reyes.
In basic, officers are asking individuals who have gentle circumstances of COVID-19 to deal with their signs at residence, as they might a chilly or flu, and chorus from in search of care at hospitals. People experiencing shortness of breath, nonetheless, ought to positively go to the emergency room, stated Blomkalns.
For kids, the standards could also be a bit completely different. Shortness of breath ought to set off a go to, as ought to altered psychological state, extreme irritability, or an incapability to eat or drink, stated Dr. Nicolaus Glomb, a pediatric emergency care doctor at UCSF Benioff Children’s Hospital.
Gov. Gavin Newsom stated Tuesday that tough projections counsel the state may need anyplace from four,000 to 20,000 further beds to deal with sufferers with critical circumstances of COVID-19.
The testing issues fear Noble, as do the tools shortages, however not almost as a lot because the potential for lots of sick folks. “I’m mostly worried about a tsunami of very ill patients that we’re not equipped to take care of,” stated Noble.
Blomkalns isn’t certain whether or not or when Stanford would possibly exceed capability, saying the caseload trajectory might hinge on how aggressively state and nationwide authorities transfer to chop off routes of group transmission. “It all depends on what happens in the coming weeks and days,” she stated. “We know what we need to do, and we’re doing the job.”
KHN Senior Correspondents JoNel Aleccia and Jenny Gold contributed to this report.