This story is a part of a partnership between NPR and Kaiser Health News.
This story may be republished free of charge (details).
Seattle mourned the information: Elizabeth and Robert Mar died of COVID-19 inside a day of one another. They would have celebrated 50 years of marriage in August.
But their deaths on the finish of March weren’t the identical. Liz, a vivacious matriarch at 72, died after two weeks sedated on a ventilator. Her analytical engineer husband, Robert, 78, selected no aggressive measures. He was in a position to talk with their grownup youngsters till almost the tip.
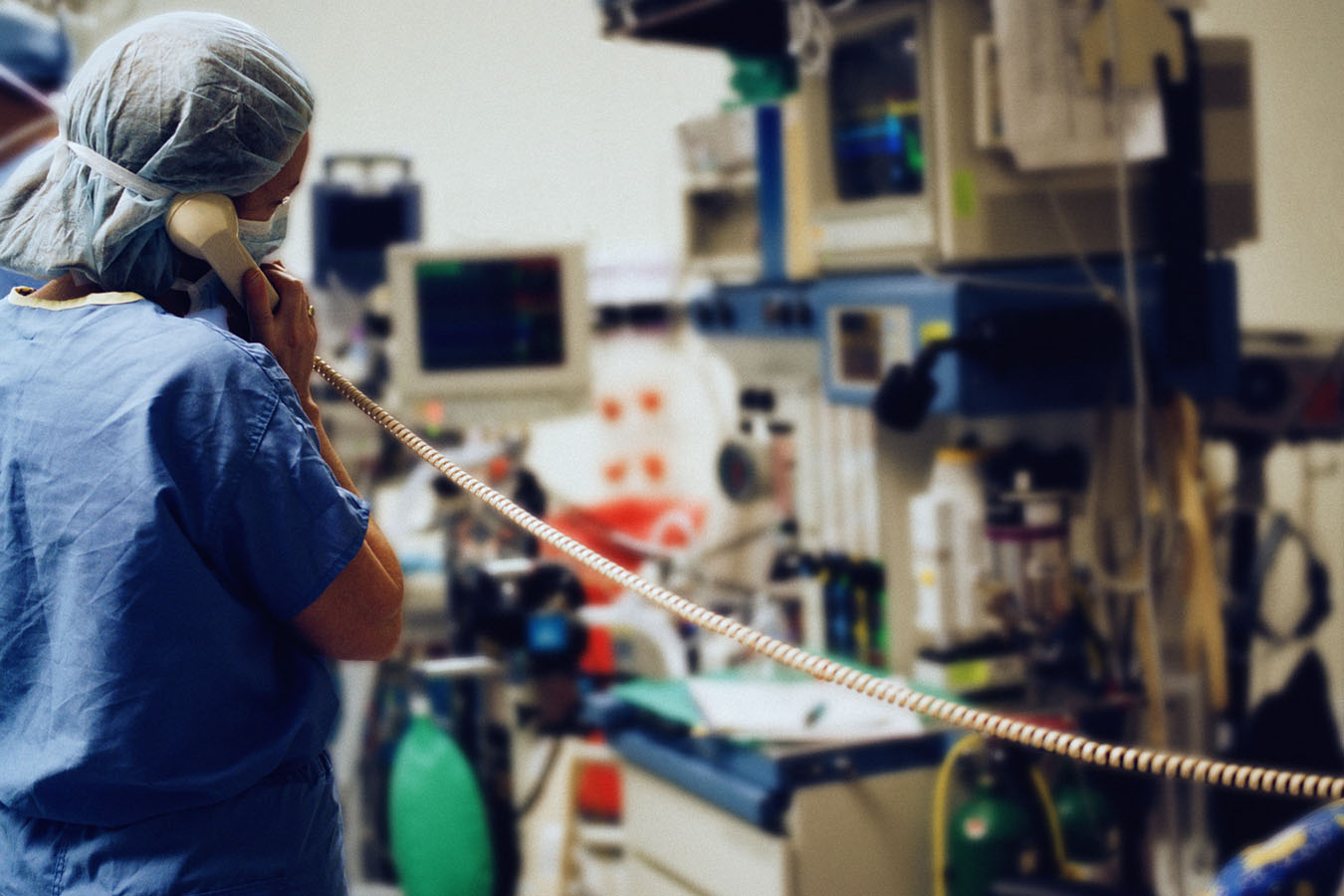
Clinician Darrell Owens helped the Mar household navigate this extremely tough time.
“You cannot underestimate the stress on family members who cannot visit and are now in a crisis mode trying to talk this through over the phone,” stated Owens, a doctor of nursing practice who runs palliative and supportive care on the University of Washington Medical Center-Northwest in Seattle.
Elizabeth and Robert Mar on their first marriage ceremony anniversary in Portland, Oregon, on Aug. 22, 1971.(Courtesy of Angie Okumoto)
Owens, like different palliative care specialists in COVID-19 sizzling spots across the nation, has seen his skilled duties remodeled by the lethal coronavirus. Patients and their households face abrupt choices in regards to the sort of care they need, and time for delicate deliberation is scarce. Conversations as soon as held in individual are actually over the cellphone, with all of the nuances of nonverbal communication misplaced. The consolation of household on the bedside of the dying is all however gone.
This is the brand new actuality for many who follow palliative medication — a speciality targeted on relieving ache and signs, enhancing high quality of life, and offering help to sufferers and households throughout extreme, power or deadly sickness.
Doctors and nurses educated on this department of medication are in high demand as hospitals deal with hundreds of terribly in poor health sufferers who might find yourself on life help with solely a small chance of survival.
“This is a horrible virus that we don’t have a cure for,” Owens stated. “As much as we are obligated to save people’s lives, we are as obligated to save their deaths.”
Before the coronavirus, Owens hardly ever labored within the emergency room. Now he’s there recurrently, referred to as in at any time when a suspected or confirmed coronavirus affected person at excessive danger of issues comes by the doorways.
“It is a totally different atmosphere in an emergency room,” Owens stated. “The conversations are more abbreviated than they would be because you are behind a mask, you are in a loud room, completely gowned up.”
Essential Conversations Under Strain
It’s a tricky option to speak by delicate and essential questions on a affected person’s likelihood of survival and what they need.
“This is completely unprecedented,” stated Dr. Diane Meier, director of the Center to Advance Palliative Care and a professor on the Icahn School of Medicine at Mount Sinai.
During the surge of coronavirus sufferers in New York City, Meier stated, her hospital system arrange a palliative care hotline for members of the family of sufferers.
Email Sign-Up
Subscribe to KHN’s free Morning Briefing.
“You can’t see their facial expression, all the cues you normally get with face-to-face communication are very hard to pick up over the phone,” Meier stated.
Nonetheless, she stated, these conversations — particularly with such a fast-moving and poorly understood virus — are a vital piece of the pandemic response.
“Palliative care specialists are a scarce resource, just like ventilators and ICU beds,” she stated.
Dr. Hope Wechkin, medical director of EvergreenHealth Hospice and Palliative Care in Kirkland, Washington, stated palliative medication is essentially about “being with patients during times of profound uncertainty, and continuing to place comfort and enhanced quality of life front and center.”
“We now have this new player [coronavirus] — as we are evaluating a patient’s goals of care,” she stated.
One Family, Two Kinds Of Death
While a lot of the nation was nonetheless waking as much as the pandemic, siblings Angie Okumoto, Rich Mar and Rob Mar have been already navigating these wrenching choices about their dad and mom’ care.
In early March, their mom, Liz, contracted the coronavirus and was admitted to the hospital.
Lively and hardworking, Liz was co-owner of the household’s fashionable Hawaiian restaurant, Kona Kitchen, which she based together with her daughter and son-in-law.
“She was one of those people that quickly made friends and made an impression on everyone,” stated her son Rich. “Young people would look to her as a grandmother figure.”
Known for her heat, she loved giving clients a hug or phrase of recommendation. Angie stated that when she and her siblings have been rising up, her dad and mom made positive that they had household dinners, and her mom introduced that very same feeling of togetherness to their eating places.
“She cared for people and wanted to know what was going on in their lives,” she stated.
Liz had been in good well being earlier than contracting the virus. When her oxygen ranges fell, her son took her to the ER.
“It was the last time I got to hear a response from her,” Rob stated. “That was the hardest part — not knowing it would be the last time.”
The hospital was nonetheless adjusting its operations to account for the wave of COVID-19 sufferers and wasn’t but particularly screening sufferers with the coronavirus about their end-of-life needs.
As she was admitted, the hospital workers requested about what sort of medical interventions she needed, if crucial. “Do you want CPR? Do you want to be put on life support?”
Their mom was weak however nonetheless aware. She stated sure. Her youngsters agreed.
“We just had no idea what this virus was going to do,” Angie stated. “We were trying to give her the opportunity to fight it.”
But their mom’s well being worsened, and shortly she was on a ventilator within the intensive care unit.
“For 14 days on the ventilator, she was alone,” Angie stated. Her brother Rob provides: “That’s the part that hurts the most, and what will haunt me forever.”
Near the tip, the three youngsters did get to go to their mom one final time.
“We were all gowned up and she was sedated,” Rich stated. “We were trying to talk to her and let her hear our voices.”
Meanwhile, their father, Robert, had additionally grow to be sick. He had been a civilian operations analyst for the Navy.
“He was on a Ph.D. track and quit his program to support his new son, me,” Rob remembered. “My dad was more of the analytical type, he could give you a practical solution for everything.”
In the early years of his marriage, Robert was supporting a family of seven, together with their grandparents. His youngsters describe him as cerebral, an ideal complement to his extra extroverted spouse.
“They really meshed well together — it worked for them,” Rich stated.
Robert was admitted to the identical hospital as his spouse. He appeared steady the primary few days. But then his oxygen ranges decreased and he began to say no.
He had been clear about his end-of-life care needs.
“From Day One, he said he did not want to be on life support,” Angie stated.
‘This Awful, Awful Truth’
Darrell Owens began managing Robert’s care. The household talked and texted with Owens. He’d give them common updates and inform them what to anticipate.
“He had to deliver this awful, awful truth, but the way he did it was so compassionate,” Angie stated. “He helped us arrange everything we needed for our dad.”
“I appreciated the honesty,” Rob stated. “I found that the most reassuring and valuable thing.”
Because he had determined towards aggressive therapy, their father was by no means moved to the ICU. He was in a position to have a couple of in-person visits together with his three youngsters. Since he wasn’t on a ventilator, they might have a dialog.
Rob stated his father’s therapy on the finish of his life was on his personal phrases: “That was very important to him.”
Owens managed Robert’s care to the very finish, and ensured that Robert might learn the previous couple of textual content messages from his son.
“They were basically goodbyes,” Rich stated.
Robert additionally shared reminiscences with Owens about his spouse and youngsters.
“My dad opened as much as him about our family,” Angie stated. “Dr. Owens knew quite a bit about us.”
The Mars are deeply grateful to the nurses and medical doctors who cared for his or her dad and mom. They perceive that hospitals are limiting guests to attenuate the prospect of an infection and protect restricted provides of masks and robes.
Still, it doesn’t cease Angie from questioning what might need been completely different if she had stated goodbye to her mom earlier than she was intubated, or had the prospect to take a seat subsequent to her whereas on the ventilator.
“What if I got to be bedside to my mom earlier, when she wasn’t heavily sedated, holding her hand and just being present,” Angie stated. “That we’ll never know.”
It’s a brand new method of experiencing dying that households are coming to know because the coronavirus retains them at a distance in these last moments.
This story is a part of NPR’s reporting partnership with Kaiser Health News.
This story is a part of a partnership between NPR and Kaiser Health News.
This story may be republished free of charge (details). Related Topics Aging Public Health States COVID-19 End Of Life Palliative Care