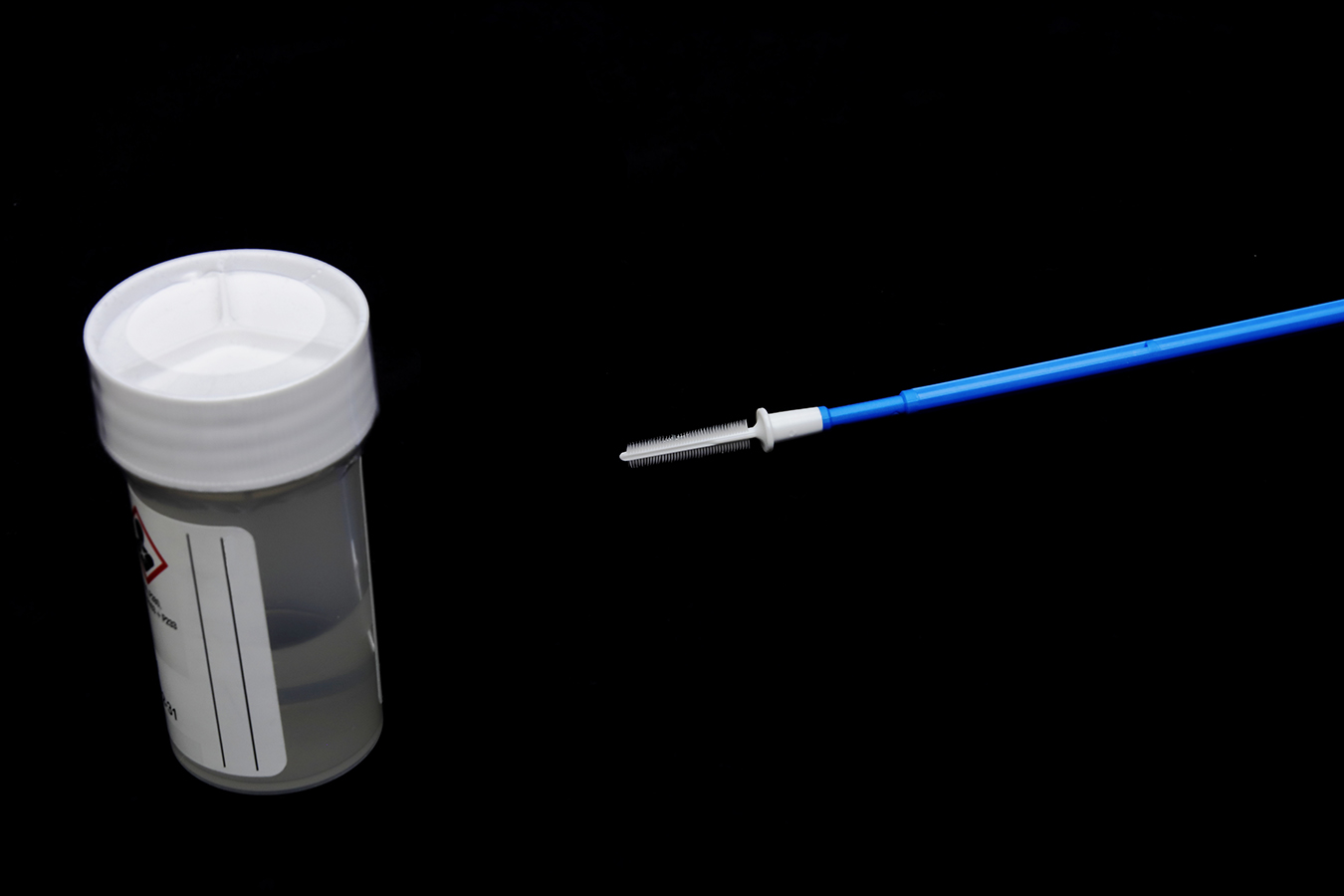
With a tiny brush, briefly swab the vagina to gather cells. Then slide the swab right into a screening package and drop it into the mail.
Proponents imagine a easy take a look at like this, which will be achieved at residence, might assist the U.S. transfer nearer to eradicating cervical most cancers. The National Cancer Institute plans to launch a multisite examine subsequent yr involving roughly 5,000 ladies to evaluate whether or not self-sampling at house is similar to screening within the workplace by a clinician.
Nearly 14,000 Americans this year shall be identified with the extremely preventable most cancers, and greater than four,000 will die. Women who’re uninsured or can’t get common medical care usually tend to miss out on lifesaving screening, stated Vikrant Sahasrabuddhe, a program director within the NCI’s Division of Cancer Prevention. If ladies may accumulate the vaginal and cervical cells to be examined for human papillomavirus (HPV) — the virus that causes nearly all cervical cancers — they may get screened from residence, simply as home-based stool samples can be utilized to detect colon most cancers, he stated.
“What we have seen is this persistent group of women who continue to get cervical cancer every year,” stated Sahasrabuddhe, who oversees research involving HPV-related cancers. “And that number is really not going down.”
Federal officers hope the analysis will fast-track a take a look at permitted by the Food and Drug Administration that might be a part of screening pointers if self-sampling is proved efficient, Sahasrabuddhe stated. Rather than look forward to self-sampling research to be achieved by the person firms that make the HPV assessments for clinicians, federal officers will group up with the businesses, tutorial establishments and others in a public-private partnership, he defined. NCI officers, who count on to spend about $6 million in federal funds, will oversee the examine’s information and evaluation.
“If every company goes and does their own trial, they may take years to achieve it,” Sahasrabuddhe stated. “We want to accelerate that process.”
HPV self-sampling, already promoted in international locations reminiscent of Australia and the Netherlands, is considered one of a number of approaches that U.S. cervical most cancers researchers are pursuing. Another key technique includes vaccinating adolescents towards HPV, which is transmitted via sexual exercise. As of 2018, nearly 54% of girls had been fully vaccinated by age 17, as had virtually 49% of boys, in response to the latest federal information. The international locations which have had higher success in lowering cervical most cancers — one evaluation predicts that Australia is on track to eliminate the disease — have emphasised HPV vaccination for adolescents.
Federal officers nonetheless advise vaccinated ladies to get often screened, because the vaccine doesn’t guard towards all of the strains that trigger cervical most cancers. But persuading some ladies to come back into the workplace for the bodily examination is usually a tricky promote.
For some, entry or value could also be a problem. Most insurance coverage cowl screening and there are additionally some public programs, however uninsured ladies who’re unaware of them might must pay for an workplace go to and take a look at. Besides, ladies can’t all the time break free from work or discover youngster care, or they could have had “negative emotions or experiences in the past with pelvic exams,” stated Rachel Winer, a professor of epidemiology on the University of Washington School of Public Health who research HPV self-sampling.
Reversing The Trend
Roughly four out of 5 ladies get often screened for cervical most cancers, however the charges peaked round 2000 and have been on a slight decline since, in response to federal information. That determine, which relies on affected person self-reporting, could also be optimistic. Another evaluation, which appeared on the medical information of 27,418 Minnesota ladies ages 30 to 65, discovered that almost 65% were up to date as of 2016, in response to the findings, printed final yr within the Journal of Women’s Health.
“Sadly, I think our data is probably more reflective of what’s happening with screening rates in our country,” stated Dr. Kathy MacLaughlin, a examine creator and researcher at Mayo Clinic in Rochester, Minnesota.
One hurdle to getting screened stands out as the complexity of the rules, MacLaughlin stated. Rather than an easy-to-remember annual examination, screenings happen at intervals of longer than a yr. A woman’s age helps decide when the HPV take a look at or a Pap smear, which collects cells from the cervix to search for precancerous adjustments, is beneficial by the U.S. Preventive Services Task Force.
“It’s just that challenge of, how do any of us remember to do something every three years or every five years?” MacLaughlin stated. “That’s hard.”
At-Home Logistics
While the NCI hasn’t but settled on the exact self-sampling strategy it’ll use, the approach usually requires the lady to insert a tiny brush into her vagina and rotate it a number of occasions to gather the cells. Then she slides the comb right into a specimen container that has a preservative answer and returns the package for HPV evaluation.
According to a assessment of research printed in 2018 within the medical journal BMJ, the accuracy of figuring out HPV was related when the samples had been collected by ladies at residence as when collected by clinicians. A urine-based HPV test, which can show simpler for girls to carry out, is also being studied, stated Jennifer Smith, a professor of epidemiology on the University of North Carolina’s Gillings School of Global Public Health.
Before firms can pursue purposes for an FDA-approved residence take a look at, self-sampling by ladies needs to be proven similar to detect HPV, although maybe it is probably not fairly as correct as when a clinician is concerned, Sahasrabuddhe stated. NCI officers are nonetheless finalizing examine particulars. But the plan is to ask 4 firms that already manufacture HPV assessments for clinicians to take part, Sahasrabuddhe stated. The firms will choose up the tab for the price of the assessments in addition to future charges associated to pursuing license purposes via the FDA, he stated. Sahasrabuddhe expects the examine outcomes to be accessible by 2024, if not sooner.
Any girl who assessments optimistic for HPV shall be referred for procedures, together with presumably a biopsy, to search for irregular cells or cervical most cancers, Sahasrabuddhe stated.
If an FDA-approved residence take a look at is developed, it’s essential that uninsured ladies and others who don’t have easy accessibility to medical care be capable to get these procedures, Smith stated.
“You just don’t send random kits out to people’s homes,” Smith stated, “and not ensure that they have someone to talk to about the results and are going to be able to be integrated into a follow-up system.”